Page 76 - JSOM Summer 2025
P. 76
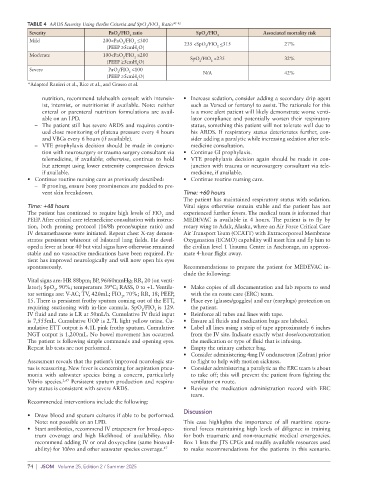
TABLE 4 ARDS Severity Using Berlin Criteria and SpO /FIO Ratio 40–42
2 2
Severity PaO /FIO ratio SpO /FIO Associated mortality risk
2 2 2 2
Mild 200<PaO /FIO ≤300
2
2
(PEEP ≥5cmH O) 235 <SpO /FIO <315 27%
2
2
2
Moderate 100<PaO /FIO ≤200
2 2 SpO /FIO <235 32%
(PEEP ≥5cmH O) 2 2
2
Severe PaO /FIO ≤100
2 2 N/A 42%
(PEEP ≥5cmH O)
2
*Adapted Ranieri et al., Rice et al., and Grasso et al.
nutrition, recommend telehealth consult with intensiv- • Increase sedation, consider adding a secondary drip agent
ist, internist, or nutritionist if available. Note: neither such as Versed or fentanyl to assist. The rationale for this
enteral or parenteral nutrition formulations are avail- is a more alert patient will likely demonstrate worse venti-
able on an LPD. lator compliance and potentially worsen their respiratory
– The patient still has severe ARDS and requires contin- status, something this patient will not tolerate well due to
ued close monitoring of plateau pressure every 4 hours his ARDS. If respiratory status deteriorates further, con-
and VBGs every 6 hours (if available). sider adding a paralytic while increasing sedation after tele-
– VTE prophylaxis decision should be made in conjunc- medicine consultation.
tion with neurosurgery or trauma surgery consultant via • Continue GI prophylaxis.
telemedicine, if available; otherwise, continue to hold • VTE prophylaxis decision again should be made in con-
but attempt using lower extremity compression devices junction with trauma or neurosurgery consultant via tele-
if available. medicine, if available.
• Continue routine nursing care as previously described: • Continue routine nursing care.
– If proning, ensure bony prominences are padded to pre-
vent skin breakdown. Time: +60 hours
The patient has maintained respiratory status with sedation.
Time: +48 hours Vital signs otherwise remain stable and the patient has not
The patient has continued to require high levels of FIO and experienced further fevers. The medical team is informed that
2
PEEP. After critical care telemedicine consultation with instruc- MEDEVAC is available in 4 hours. The patient is to fly by
tion, both proning protocol (16/8h prone/supine ratio) and rotary wing to Adak, Alaska, where an Air Force Critical Care
IV dexamethasone were initiated. Repeat chest X-ray demon- Air Transport Team (CCATT) with Extracorporeal Membrane
strates persistent whiteout of bilateral lung fields. He devel- Oxygenation (ECMO) capability will meet him and fly him to
oped a fever at hour 40 but vital signs have otherwise remained the civilian level 1 Trauma Center in Anchorage, an approxi-
stable and no vasoactive medications have been required. Pa- mate 4-hour flight away.
tient has improved neurologically and will now open his eyes
spontaneously. Recommendations to prepare the patient for MEDEVAC in-
clude the following:
Vital signs are: HR 88bpm; BP, 96/60mmHg; RR, 20 (on venti-
lator); SpO , 90%; temperature 39°C; RASS, 0 to +1. Ventila- • Make copies of all documentation and lab reports to send
2
tor settings are: V-AC; TV, 420mL; FIO , 70%; RR, 18; PEEP, with the en route care (ERC) team.
2
15. There is persistent frothy sputum coming out of the ETT, • Place eye (glasses/goggles) and ear (earplugs) protection on
requiring suctioning with in-line cannula. SpO /FIO is 129. the patient.
2
2
IV fluid and rate is LR at 50mL/h. Cumulative IV fluid input • Reinforce all tubes and lines with tape.
is 7,555mL. Cumulative UOP is 2.7L light yellow urine. Cu- • Ensure all fluids and medication bags are labeled.
mulative ETT output is 4.1L pink frothy sputum. Cumulative • Label all lines using a strip of tape approximately 6 inches
NGT output is 1,200mL. No bowel movement has occurred. from the IV site. Indicate exactly what dose/concentration
The patient is following simple commands and opening eyes. the medication or type of fluid that is infusing.
Repeat lab tests are not performed. • Empty the urinary catheter bag.
• Consider administering 4mg IV ondansetron (Zofran) prior
Assessment reveals that the patient’s improved neurologic sta- to flight to help with motion sickness.
tus is reassuring. New fever is concerning for aspiration pneu- • Consider administering a paralytic as the ERC team is about
monia with saltwater species being a concern, particularly to take off; this will prevent the patient from fighting the
Vibrio species. 2,47 Persistent sputum production and respira- ventilator en route.
tory status is consistent with severe ARDS. • Review the medication administration record with ERC
team.
Recommended interventions include the following:
Discussion
• Draw blood and sputum cultures if able to be performed.
Note: not possible on an LPD. This case highlights the importance of all maritime opera-
• Start antibiotics, recommend IV ertapenem for broad-spec- tional forces maintaining high levels of diligence in training
trum coverage and high likelihood of availability. Also for both traumatic and non-traumatic medical emergencies.
recommend adding IV or oral doxycycline (same bioavail- Box 1 lists the JTS CPGs and readily available resources used
ability) for Vibro and other seawater species coverage. 47 to make recommendations for the patients in this scenario.
74 | JSOM Volume 25, Edition 2 / Summer 2025