Page 74 - JSOM Summer 2025
P. 74
• Maintain a RASS (Richmond Agitation and Sedation Score) • Extremity injuries take last priority in critically ill patients
of 0, if possible, to assist with neurologic exams (Table 3). 31 unless there is neurovascular compromise; if identified
during the primary or secondary survey, the limb should be
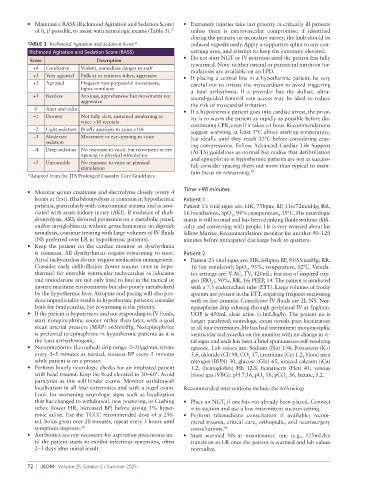
TABLE 3 Richmond Agitation and Sedation Score 30 reduced expeditiously. Apply a supportive splint to any con-
Richmond Agitation and Sedation Score (RASS) cerning area, and attempt to keep the extremity elevated.
Score Description • Do not start NGT or IV nutrition until the patient has fully
+4 Combative Violent, immediate danger to staff rewarmed. Note: neither enteral or parenteral nutrition for-
mulations are available on an LPD.
+3 Very agitated Pulls at or removes tubes, aggressive • If placing a central line in a hypothermic patient, be very
+2 Agitated Frequent non-purposeful movements, careful not to irritate the myocardium to avoid triggering
fights ventilator a fatal arrhythmia. If a provider has the skillset, ultra-
+1 Restless Anxious, apprehensive but movements not sound-guided femoral vein access may be ideal to reduce
aggressive the risk of myocardial irritation.
0 Alert and calm • If a hypothermic patient goes into cardiac arrest, the prior-
–1 Drowsy Not fully alert, sustained awakening to ity is to warm the patient as rapidly as possible before dis-
voice >10 seconds continuing CPR, even if it takes >1 hour. Recommendations
–2 Light sedation Briefly awakens to voice <10s suggest warming at least 5°C above starting temperature,
–3 Moderate Movement or eye-opening to voice but ideally until they reach 32°C before considering ceas-
sedation ing compressions. Follow Advanced Cardiac Life Support
–4 Deep sedation No response to voice, but movement or eye (ACLS) guidelines as normal but realize that defibrillation
opening to physical stimulation
–5 Unrousable No response to voice or physical and epinephrine in hypothermic patients are not as success-
stimulation ful; consider spacing them out more than typical to main-
39
*Adapted from the JTS Prolonged Casualty Care Guidelines. tain focus on rewarming.
Time +90 minutes
• Monitor serum creatinine and electrolytes closely (every 4
hours at first). Rhabdomyolysis is common in hypothermic Patient 1
patients, particularly with concomitant trauma and is asso- Patient 1’s vital signs are: HR, 75bpm; BP, 116/72mmHg; RR,
ciated with acute kidney injury (AKI). If evidence of rhab- 16 breaths/min, SpO , 94%; temperature, 35°C. His neurologic
2
domyolysis, AKI, elevated potassium on a metabolic panel, status is still normal and has been drinking fluids without diffi-
and/or myoglobinuria without gross hematuria on dipstick culty and conversing with people. He is very worried about his
urinalysis, continue treating with large volumes of IV fluids fellow Marine. Recommendation: monitor for another 90–120
(NS preferred over LR in hypothermic patients). minutes before anticipated discharge back to quarters.
• Keep the patient on the cardiac monitor as dysrhythmia
is common. All dysrhythmias require rewarming to treat. Patient 2
Atrial tachycardias do not require medication management. • Patient 2’s vital signs are: HR, 64bpm; BP, 95/55mmHg; RR,
Consider early defibrillation (lower success rates in hypo- 16 (on ventilator); SpO , 95%; temperature, 32°C. Ventila-
2
thermia) for unstable ventricular tachycardias as lidocaine tor settings are: V-AC, TV, 420mL; fraction of inspired oxy-
and amiodarone are not only hard to find in the tactical or gen (FIO ), 90%; RR, 16; PEEP, 14. The patient is intubated
2
austere maritime environments but also poorly metabolized with a 7.5 endotracheal tube (ETT). Large volumes of frothy
by the hypothermic liver. Atropine and pacing will also pro- sputum are present in the ETT, requiring frequent suctioning
duce unpredictable results in hypothermic patients; consider with in-line cannula. Cumulative IV fluids are 2L NS. Nor-
both for bradycardia, but rewarming is the priority. epinephrine drip infusing through peripheral IV at 5µg/min.
• If the patient is hypotensive and not responding to IV fluids, UOP is 450mL clear urine (>1mL/kg/h). The patient no is
start norepinephrine sooner rather than later, with a goal longer paralyzed; neurologic exam reveals pain localization
mean arterial pressure (MAP) >65mmHg. Norepinephrine in all four extremities. He has had intermittent monomorphic
is preferred to epinephrine in hypothermic patients as it is ventricular tachycardia on the monitor with no change in vi-
the least arrhythmogenic. tal signs and each has been a brief spontaneous self-resolving
• Norepinephrine (Levophed) drip range: 2–20µg/min, titrate episode. Lab values are: Sodium (Na) 134, Potassium (K+)
every 3–5 minutes as needed, reassess BP every 5 minutes 5.6, chloride (Cl) 98, CO 17, creatinine (Cr) 1.2, blood urea
2
while patient is on a pressor. nitrogen (BUN) 30, glucose (Glu) 65, ionized calcium (iCa)
• Perform hourly neurologic checks for an intubated patient 1.2, (hemoglobin) Hb 12.8, hematocrit (Hct) 41; venous
with head trauma. Keep the head elevated to 30–60°. Avoid blood gas (VBG): pH 7.16, pO 16, pCO 36, lactate, 5.2.
2
2
paralytics as this will hinder exams. Monitor withdrawal/
localization in all four extremities and with a pupil exam. Recommended interventions include the following:
Look for worsening neurologic signs such as localization
that has changed to withdrawal, new posturing, or Cushing • Place an NGT, if one has not already been placed. Connect
reflex (lower HR, increased BP) before giving 3% hyper- it to suction and use a low intermittent suction setting.
tonic saline. Use the TCCC recommended dose of a 250- • Perform telemedicine consultation if available; recom-
mL bolus given over 20 minutes, repeat every 3 hours until mend trauma, critical care, orthopedic, and neurosurgery
symptoms improve. 38 consultations. 40
• Antibiotics are not necessary for aspiration pneumonia un- • Start warmed NS at maintenance rate (e.g., 125mL/h);
til the patient starts to exhibit infectious symptoms, often transition to LR once the patient is warmed and lab values
2–3 days after initial insult. normalize.
72 | JSOM Volume 25, Edition 2 / Summer 2025