Page 83 - JSOM Spring 2023
P. 83
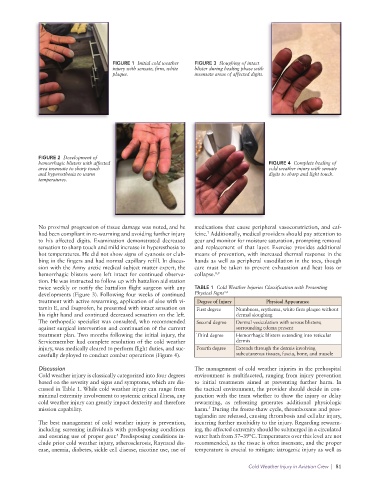
FIGURE 1 Initial cold weather FIGURE 3 Sloughing of intact
injury with sensate, firm, white blister during healing phase with
plaque. insensate areas of affected digits.
FIGURE 2 Development of
hemorrhagic blisters with affected FIGURE 4 Complete healing of
area insensate to sharp touch cold weather injury with sensate
and hyperesthesia to warm digits to sharp and light touch.
temperatures.
No proximal progression of tissue damage was noted, and he medications that cause peripheral vasoconstriction, and caf-
had been compliant in re-warming and avoiding further injury feine. Additionally, medical providers should pay attention to
7
to his affected digits. Examination demonstrated decreased gear and monitor for moisture saturation, prompting removal
sensation to sharp touch and mild increase in hyperesthesia to and replacement of that layer. Exercise provides additional
hot temperatures. He did not show signs of cyanosis or club- means of prevention, with increased thermal response in the
bing in the fingers and had normal capillary refill. In discus- hands as well as peripheral vasodilation in the toes, though
sion with the Army arctic medical subject matter expert, the care must be taken to prevent exhaustion and heat loss or
hemorrhagic blisters were left intact for continued observa- collapse. 8,9
tion. He was instructed to follow up with battalion aid station
twice weekly or notify the battalion flight surgeon with any TABLE 1 Cold Weather Injuries Classification with Presenting
developments (Figure 3). Following four weeks of continued Physical Signs 5,6
treatment with active rewarming, application of aloe with vi- Degree of Injury Physical Appearance
tamin E, and ibuprofen, he presented with intact sensation on First degree Numbness, erythema, white firm plaque without
his right hand and continued decreased sensation on the left. dermal sloughing
The orthopedic specialist was consulted, who recommended Second degree Dermal vesiculation with serous blisters;
against surgical intervention and continuation of the current surrounding edema present
treatment plan. Two months following the initial injury, the Third degree Hemorrhagic blisters extending into reticular
Servicemember had complete resolution of the cold weather dermis
injury, was medically cleared to perform flight duties, and suc- Fourth degree Extends through the dermis involving
cessfully deployed to conduct combat operations (Figure 4). subcutaneous tissues, fascia, bone, and muscle
Discussion The management of cold weather injuries in the prehospital
Cold weather injury is classically categorized into four degrees environment is multifaceted, ranging from injury prevention
based on the severity and signs and symptoms, which are dis- to initial treatments aimed at preventing further harm. In
cussed in Table 1. While cold weather injury can range from the tactical environment, the provider should decide in con-
minimal extremity involvement to systemic critical illness, any junction with the team whether to thaw the injury or delay
cold weather injury can greatly impact dexterity and therefore rewarming, as refreezing generates additional physiologic
5
mission capability. harm. During the freeze-thaw cycle, thromboxane and pros-
taglandin are released, causing thrombosis and cellular injury,
The best management of cold weather injury is prevention, incurring further morbidity to the injury. Regarding rewarm-
including screening individuals with predisposing conditions ing, the affected extremity should be submerged in a circulated
5
and ensuring use of proper gear. Predisposing conditions in- water bath from 37–39°C. Temperatures over this level are not
clude prior cold weather injury, atherosclerosis, Raynaud dis- recommended, as the tissue is often insensate, and the proper
ease, anemia, diabetes, sickle cell disease, nicotine use, use of temperature is crucial to mitigate iatrogenic injury as well as
Cold Weather Injury in Aviation Crew | 81