Page 116 - JSOM Winter 2022
P. 116
combat-related injuries from 2003 until 2015. We observed were found to be independent risk factors associated with
no changes in the proportion of patients who died of ARDS, development of ARDS. That study also noted an association
suggesting there was not an overall improvement in ARDS between plasma transfusions and severe chest trauma with
survival over time, which would have confounded the prior worsening severity of ARDS. 13
analyses (Figure 1).
Trauma-associated ARDS is challenging and is a distinct entity
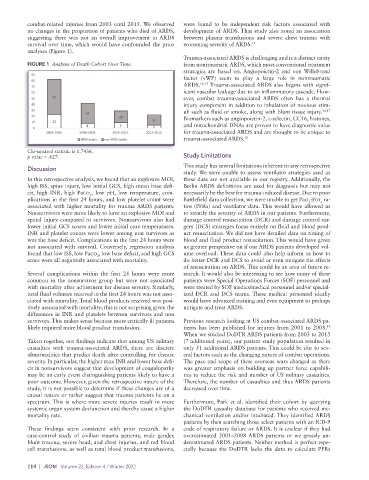
FIGURE 1 Analysis of Death Cohort Over Time. from nontraumatic ARDS, which most conventional treatment
strategies are based on. Angiopoietin-2 and von Willebrand
factor (vWF) seem to play a large role in nontraumatic
ARDS. 14,15 Trauma-associated ARDS also begins with signif-
icant vascular leakage due to an inflammatory cascade. How-
ever, combat trauma-associated ARDS often has a thermal
injury component in addition to inhalation of noxious stim-
uli such as fluid or smoke, along with blunt tissue injury. 16,17
Biomarkers such as angiopoietin-2, l-selectin, CC16, histones,
and mitochondrial DNAs are proven to have diagnostic value
for trauma-associated ARDS and are thought to be unique to
trauma-associated ARDS. 18
Chi-squared statistic is 1.7436.
p value = .627. Study Limitations
This study has several limitations inherent to any retrospective
Discussion
study. We were unable to assess ventilator strategies used as
In this retrospective analysis, we found that an explosive MOI, these data are not available in our registry. Additionally, the
high ISS, spine injury, low initial GCS, high mean base defi- Berlin ARDS definitions are used for diagnosis but may not
cit, high INR, high Paco , low pH, low temperature, com- necessarily be the best for trauma-induced disease. Due to poor
2
plications in the first 24 hours, and low platelet count were battlefield data collection, we were unable to get Pao :Fio ra-
2
2
associated with higher mortality for trauma ARDS patients. tios (PFRs) and ventilator data. This would have allowed us
Nonsurvivors were more likely to have an explosive MOI and to stratify the severity of ARDS in our patients. Furthermore,
spinal injury compared to survivors. Nonsurvivors also had damage control resuscitation (DCR) and damage control sur-
lower initial GCS scores and lower initial core temperatures. gery (DCS) strategies focus entirely on fluid and blood prod-
INR and platelet counts were lower among non survivors as uct resuscitation. We did not have detailed data on timing of
was the base deficit. Complications in the first 24 hours were blood and fluid product resuscitation. This would have given
not associated with survival. Conversely, regression analysis us greater perspective on if our ARDS patients developed vol-
found that low ISS, low Paco , low base deficit, and high GCS ume overload. These data could also help inform us how to
2
score were all negatively associated with mortality. do better DCR and DCS to avoid or even mitigate the effects
of resuscitation on ARDS. This could be an area of future re-
Several complications within the first 24 hours were more search. It would also be interesting to see how many of these
common in the nonsurvivor group but were not associated patients were Special Operations Forces (SOF) personnel and
with mortality after adjustment for disease severity. Similarly, were treated by SOF medics/medical personnel and/or special-
total fluid volumes received in the first 24 hours was not asso- ized DCR and DCS teams. These medical personnel ideally
ciated with mortality. Total blood products received was posi- would have advanced training and even equipment to perhaps
tively associated with mortality; this is not surprising given the mitigate and treat ARDS.
differences in INR and platelets between survivors and non
survivors. This makes sense because more critically ill patients Previous research looking at US combat-associated ARDS pa-
likely required more blood product transfusion. tients has been published for injuries from 2001 to 2008.
19
When we studied DoDTR ARDS patients from 2003 to 2015
Taken together, our findings indicate that among US military (7 additional years), our patient study population resulted in
casualties with trauma-associated ARDS, there are discrete only 51 additional ARDS patients. This could be due to sev-
abnormalities that predict death after controlling for disease eral factors such as the changing nature of combat operations.
severity. In particular, the higher max INR and lower base defi- The pace and scope of these overseas wars changed as there
cit in nonsurvivors suggest that development of coagulopathy was greater emphasis on building up partner force capabili-
may be an early event distinguishing patients likely to have a ties to reduce the risk and number of US military casualties.
poor outcome. However, given the retrospective nature of the Therefore, the number of casualties and thus ARDS patients
study, it is not possible to determine if these changes are of a decreased over time.
causal nature or rather suggest that trauma patients lie on a
spectrum. This is where more severe injuries result in more Furthermore, Park et al. identified their cohort by querying
systemic organ system dysfunction and thereby cause a higher the DoDTR casualty database for patients who received me-
mortality rate. chanical ventilation and/or intubated. They identified ARDS
patients by then searching those select patients with an ICD-9
These findings seem consistent with prior research. In a code of respiratory failure or ARDS. It is unclear if they had
case-control study of civilian trauma patients, male gender, overestimated 2001–2008 ARDS patients or we grossly un-
blunt trauma, severe head, and chest injuries, and red blood derestimated ARDS patients. Neither method is perfect espe-
cell transfusions, as well as total blood product transfusions, cially because the DoDTR lacks the data to calculate PFRs
114 | JSOM Volume 22, Edition 4 / Winter 2022