Page 71 - JSOM Fall 2022
P. 71
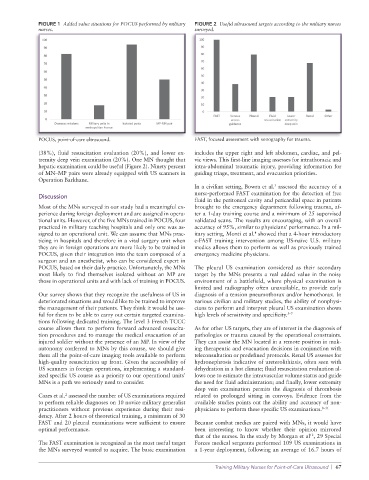
FIGURE 1 Added value situations for POCUS performed by military FIGURE 2 Useful ultrasound targets according to the military nurses
nurses. surveyed.
POCUS, pointofcare ultrasound. FAST, focused assessment with sonography for trauma.
(38%), fluid resuscitation evaluation (20%), and lower ex includes the upper right and left abdomen, cardiac, and pel
tremity deep vein examination (20%). One MN thought that vic views. This firstline imaging assesses for intrathoracic and
hepatic examination could be useful (Figure 2). Ninety percent intraabdominal traumatic injury, providing information for
of MN–MP pairs were already equipped with US scanners in guiding triage, treatment, and evacuation priorities.
Operation Barkhane.
In a civilian setting, Bowra et al. assessed the accuracy of a
3
nurseperformed FAST examination for the detection of free
Discussion
fluid in the peritoneal cavity and pericardial space in patients
Most of the MNs surveyed in our study had a meaningful ex brought to the emergency department following trauma, af
perience during foreign deployment and are assigned in opera ter a 1day training course and a minimum of 25 supervised
tional units. However, of the five MNs trained in POCUS, four validated scans. The results are encouraging, with an overall
practiced in military teaching hospitals and only one was as accuracy of 95%, similar to physicians’ performance. In a mil
4
signed to an operational unit. We can assume that MNs prac itary setting, Monti et al. showed that a 4hour introductory
ticing in hospitals and therefore in a vital surgery unit when eFAST training intervention among USnaïve U.S. military
they are in foreign operations are more likely to be trained in medics allows them to perform as well as previously trained
POCUS, given their integration into the team composed of a emergency medicine physicians.
surgeon and an anesthetist, who can be considered expert in
POCUS, based on their daily practice. Unfortunately, the MNs The pleural US examination considered as their secondary
most likely to find themselves isolated without an MP are target by the MNs presents a real added value in the noisy
those in operational units and with lack of training in POCUS. environment of a battlefield, where physical examination is
limited and radiography often unavailable, to provide early
Our survey shows that they recognize the usefulness of US in diagnosis of a tension pneumothorax and/or hemothorax. In
deteriorated situations and would like to be trained to improve various civilian and military studies, the ability of nonphysi
the management of their patients. They think it would be use cians to perform and interpret pleural US examination shows
ful for them to be able to carry out certain targeted examina high levels of sensitivity and specificity. 5–7
tions following dedicated training. The level 3 French TCCC
course allows them to perform forward advanced resuscita As for other US targets, they are of interest in the diagnosis of
tion procedures and to manage the medical evacuation of an pathologies or trauma caused by the operational constraints.
injured soldier without the presence of an MP. In view of the They can assist the MN located in a remote position in mak
autonomy conferred to MNs by this course, we should give ing therapeutic and evacuation decisions in conjunction with
them all the pointofcare imaging tools available to perform teleconsultation or predefined protocols. Renal US assesses for
highquality resuscitation up front. Given the accessibility of hydronephrosis indicative of ureterolithiasis, often seen with
US scanners in foreign operations, implementing a standard dehydration in a hot climate; fluid resuscitation evaluation al
ized specific US course as a priority to our operational units’ lows one to estimate the intravascular volume status and guide
MNs is a path we seriously need to consider. the need for fluid administration; and finally, lower extremity
deep vein examination permits the diagnosis of thrombosis
2
Cazes et al. assessed the number of US examinations required related to prolonged sitting in convoys. Evidence from the
to perform reliable diagnoses on 10 novice military generalist available studies points out the ability and accuracy of non
practitioners without previous experience during their resi physicians to perform these specific US examinations. 8–11
dency. After 2 hours of theoretical training, a minimum of 30
FAST and 20 pleural examinations were sufficient to ensure Because combat medics are paired with MNs, it would have
optimal performance. been interesting to know whether their opinion mirrored
that of the nurses. In the study by Morgan et al , 29 Special
12
The FAST examination is recognized as the most useful target Forces medical sergeants performed 109 US examinations in
the MNs surveyed wanted to acquire. The basic examination a 1year deployment, following an average of 16.7 hours of
Training Military Nurses for Point-of-Care Ultrasound | 67