Page 110 - JSOM Summer 2022
P. 110
Diagnostics Treatments
There is a wide range of diagnostic equipment available to All three conditions share the same treatment goals and prin-
the SOF medic to help diagnose and guide the treatment of ciples, with the aim of effectively oxygenating the patient by
patients with BLI, inhalation injury and ARDS, particularly counteracting pulmonary edema, atelectasis and infections.
in the PFC setting. In this section, and in the following one This is accomplished through two primary means: the use
concerning treatment, there will be many ranges and values of positive pressure ventilations with positive end expiratory
listed to help drive the treatment of these critically ill patients. pressure (PEEP), and low tidal volumes (TV) to protect the
The authors would like to emphasize that it is important for lungs. As the patient’s alveoli collapse, some undergo an irre-
any provider to never let numbers on diagnostic tools over- versible collapse while others can be “recruited,” or essentially
rule their clinical assessment of the patient’s condition. Use reinflated, in order to increase oxygen diffusion. This is done
these numbers as a guide, but always treat your patient, not through properly ventilating the patient and through the use
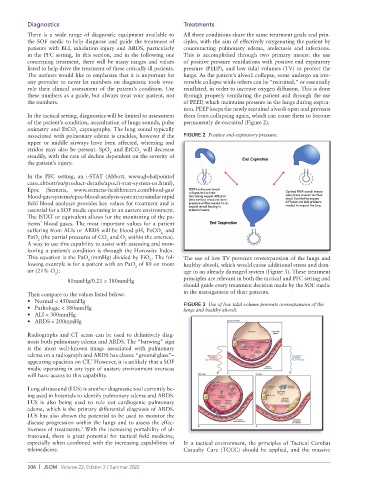
the numbers. of PEEP, which maintains pressure in the lungs during expira-
tion. PEEP keeps the newly recruited alveoli open and prevents
In the tactical setting, diagnostics will be limited to assessment them from collapsing again, which can cause them to become
of the patient’s condition, auscultation of lungs sounds, pulse permanently de-recruited (Figure 2).
oximetry and EtCO capnography. The lung sound typically
2
associated with pulmonary edema is crackles, however if the FIGURE 2 Positive end-expiratory pressure.
upper or middle airways have been affected, wheezing and
stridor may also be present. SpO and EtCO will decrease
2
2
steadily, with the rate of decline dependent on the severity of
the patient’s injury.
In the PFC setting, an i-STAT (Abbott, www.globalpointof
care.abbott/en/product-details/apoc/i-stat-system-us.html),
Epoc (Siemens, www.siemens-healthineers.com/blood-gas/
blood-gas-systems/epoc-blood-analysis-system) or similar rapid
field blood analyzer provides key values for treatment and is
essential for a SOF medic operating in an austere environment.
The ISTAT or equivalent allows for the monitoring of the pa-
tients’ blood gases. The most important values for a patient
suffering from ALIs or ARDS will be blood pH, PaCO and
2,
PaO (the partial pressures of CO and O within the arteries).
2
2
2
A way to use this capability to assist with assessing and mon-
itoring a patient’s condition is through the Horowitz Index.
This equation is the PaO (mmHg) divided by FiO . The fol- The use of low TV prevents overexpansion of the lungs and
2
2
lowing example is for a patient with an PaO of 80 on room healthy alveoli, which would cause additional stress and dam-
2
air (21% O ): age to an already damaged system (Figure 3). These treatment
2
80mmHg/0.21 = 380mmHg principles are relevant in both the tactical and PFC setting and
should guide every treatment decision made by the SOF medic
Then compare to the values listed below: in the management of their patients.
• Normal < 450mmHg
• Pathologic < 380mmHg FIGURE 3 Use of low tidal volume prevents overexpansion of the
lungs and healthy alveoli.
• ALI < 300mmHg
• ARDS < 200mmHg
Radiographs and CT scans can be used to definitively diag-
nosis both pulmonary edema and ARDS. The “batwing” sign
is the most well-known image associated with pulmonary
edema on a radiograph and ARDS has classic “ground glass”–
7
appearing opacities on CT. However, it is unlikely that a SOF
medic operating in any type of austere environment overseas
will have access to this capability.
Lung ultrasound (LUS) is another diagnostic tool currently be-
ing used in hospitals to identify pulmonary edema and ARDS.
LUS is also being used to rule out cardiogenic pulmonary
edema, which is the primary differential diagnosis of ARDS.
LUS has also shown the potential to be used to monitor the
disease progression within the lungs and to assess the effec-
tiveness of treatments. With the increasing portability of ul-
3
trasound, there is great potential for tactical field medicine,
especially when combined with the increasing capabilities of In a tactical environment, the principles of Tactical Combat
telemedicine. Casualty Care (TCCC) should be applied, and the massive
106 | JSOM Volume 22, Edition 2 / Summer 2022