Page 85 - JSOM Winter 2019
P. 85
TABLE 3 Pharmacokinetics Summary Statistics resource-constrained environments, the usual IV route of infu-
Route, Median (IQR) sion may not be reasonable, leading to delay in the administra-
IV Group IO Group IM Group tion of TXA, a drug that has been shown to be most effective
(n = 5) (n = 5) (n = 5) p when given early after traumatic injuries. IM autoinjectors
9
147.8 119.6 39.4 are an attractive modality due to the ease with which TXA
C max (μg/mL) (139.0–222.6) (88.0–121.6) (37.8–39.9) .005 could be rapidly administered in the field, potentially by non-
Time to C max 5.0 5.0 60.0 .003 medical first responders. The IM route maintains a similar
(min) (5.0–10.0) (5.0–5.0) (30.0–60.0) half-life and TXA serum concentration after 60 minutes com-
Half-life 215.5 159.2 162.5 pared with IV and IO administration, which may be useful in
(min) (180.6–807.0) (128.9–163.6) (90.8–242.7) .275 the battlefield and during prolonged evacuation times. Addi-
Area under 10,641.8 8,350.7 7,811.8 tionally, this slow absorption may also prevent the hypoten-
curve (9,518.1– (7,211.0– (6,800.6– .164 sion that has been reported with rapid administration of TXA
(μg*min/mL) 10,878.4) 10,344.5) 9,369.8) at rates greater than 100mg/min IV. In our study, we did not
20
observe any cardiovascular collapse in the five animals who
25
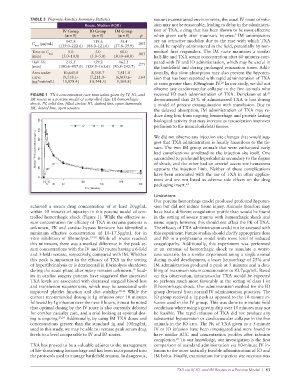
FIGURE 1 TXA concentration over time when given by IV, IO, and received IO push administration of TXA. Derickson et al.
IM routes in a porcine model of controlled class III hemorrhagic demonstrated that 25% of administered TXA is lost during
shock. IV, solid line, filled circles; IO, dashed line, open diamonds; a model of porcine exsanguination with transfusion. Due to
IM, dotted line, open squares.
the delayed absorption, IM administration of TXA may re-
duce drug loss from ongoing hemorrhage and provide lasting
biological activity that may increase as resuscitation improves
perfusion to the musculoskeletal tissues.
We did not observe any injection site changes that would sug-
gest that TXA administration is locally hazardous to the tis-
sues. The two IM group animals that were euthanized early
had complications unrelated to the injection site itself. One
succumbed to profound hyperkalemia secondary to the degree
of shock, and the other had an arterial access site hematoma
opposite the injection limb. Neither of these complications
have been associated with the use of TXA in other applica-
tions and are not listed as adverse side effects on the drug
packaging insert. 23
Limitations
Our porcine hemorrhage model produced profound hypoten-
achieved a serum drug concentration of at least 20μg/mL sion but did not induce tissue injury. Animals therefore may
within 10 minutes of injection in this porcine model of con- have had a different coagulation profile than would be found
trolled hemorrhagic shock (Figure 1). While the effective se- in the setting of severe trauma with hemorrhagic shock and
rum concentration for efficacy of TXA in trauma patients is tissue injury; however, this should not affect the PK of TXA.
unknown, PK and cardiac bypass literature has identified a The efficacy of TXA administration could not be assessed with
minimum effective concentration of 10–17.5μg/mL for in this experiment. Future studies should clarify appropriate dose
vitro inhibition of fibrinolysis. 15–18 While all routes reached and PD in a polytrauma model with some level of induced
this minimum, there was a marked difference in the peak se- coagulopathy. Additionally, this experiment was performed
rum concentrations with the IV and IO routes having a 6-fold at an extreme of hemorrhagic shock to simulate a worst-
and 3-fold increase, respectively, compared with IM. Whether case scenario. In a similar experiment using a single animal
this peak is important in the efficacy of TXA in the setting during model development, a lesser hemorrhage of 25% and
of hyperfibrinolysis or is detrimental in fibrinolysis shutdown IM administration produced a peak at 5 minutes and a dou-
during the acute phase after injury remains unknown. Stud- bling of maximum serum concentration to 83.7μcg/mL. Based
19
ies in cardiac surgery patients have suggested that increased on this observation, intramuscular TXA would be expected
TXA levels are associated with decreased surgical blood loss to perform much more favorably in the setting of class I or
and transfusion requirements, which may be associated with II hemorrhagic shock. Our administration method for the IO
improved platelet function and clot stability. 20–22 While the group deviated from normal IV administration practices. The
current recommended dosing is 1g infusion over 10 minutes IO group received a 1g push as opposed to the 10-minute in-
followed by 1g infusion over the next 8 hours, it must be noted fusion used in the IV group. This was done to simulate field
that optimal dosing by the IV route is also currently debated conditions where using a gravity drip over 10 minutes may not
for combat casualty care, and a trial looking at optimal dos- be feasible. The rapid infusion of TXA did not produce any
ing is ongoing. 23,24 Additionally, by using IM TXA doses and substantial hypotension or cardiovascular collapse in the five
concentrations greater than the standard 1g and 100mg/mL animals in the IO arm. The PK of TXA given as a 5- minute
used in this study, we may be able to increase peak serum drug IV or IO infusion have been investigated and were found to
levels to a level comparable to IV and IO routes. have similar AUC and concentration profiles after infusion
completion. To our knowledge, our investigation is the first
26
TXA has proved to be a valuable adjunct to the management comparison of standard administration via 10-minute IV in-
of life-threatening hemorrhage and has been incorporated into fusion to the more tactically feasible administration of IO and
the protocols used to manage battlefield trauma. In dangerous, IM bolus. Finally, examination for injection site necrosis was
TXA via IV, IO, and IM Routes in a Porcine Model | 83