Page 110 - JSOM Winter 2018
P. 110
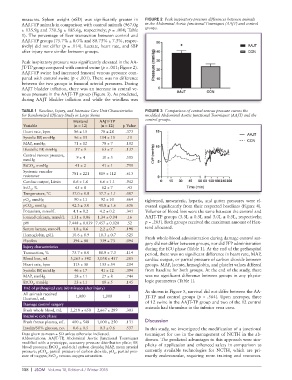
measures. Spleen weight (±SD) was significantly greater in FIGURE 2 Peak inspiratory pressure differences between animals
AAJT-TP animals in comparison with control animals (967.0g in the Abdominal Aortic Junctional Tourniquet (AAJT) and control
± 135.9g and 750.5g ± 185.6g, respectively; p = .004; Table groups.
1). The percentage of liver transection between control and
AAJT-TP groups (75.7% ± 8.0% and 80.73% ± 7.3%, respec-
tively) did not differ (p = .114). Lactate, heart rate, and SBP
after injury were similar between groups.
Peak inspiratory pressure was significantly elevated in the AA-
JT-TP group compared with control swine (p < .001; Figure 2).
AAJT-TP swine had increased femoral venous pressure com-
pared with control swine (p < .001). There was no difference
between the two groups in femoral arterial pressures. During
AAJT bladder inflation, there was an increase in central ve-
nous pressure in the AAJT-TP group (Figure 3). As predicted,
during AAJT bladder inflation and while the windlass was
TABLE 1 Baseline, Injury, and Intensive Care Unit Characteristics FIGURE 3 Comparison of central venous pressure curves the
for Randomized Efficacy Study in Large Swine modified Abdominal Aortic Junctional Tourniquet (AAJT) and the
Hextend AAJT-TP control groups.
Variable (n = 12) (n = 12) p Value
Heart rate, bpm 86 ± 15 78 ± 28 .373
Systolic BP, mmHg 96 ± 15 104 ± 10 .11
MAP, mmHg 71 ± 12 78 ± 7 .102
Diastolic BP, mmHg 57 ± 9 63 ± 7 .137
Central venous pressure, 9 ± 4 10 ± 3 .505
mmHg
EtCO , mmHg 41 ± 2 41 ± 1 .759
2
Systemic vascular
resistance 781 ± 221 819 ± 112 .613
Cardiac output, L/min 6.6 ± 1.6 6.6 ± 1.1 .942
SvO , % 65 ± 8 62 ± 7 .43
2
Temperature, °C 37.0 ± 0.8 37.7 ± 1.1 .087
pO , mmHg 90 ± 11 92 ± 10 .664 tightened, mesenteric, hepatic, and gutter pressures were el-
2
pCO , mmHg 42.3 ± 3.0 41.8 ± 1.6 .636 evated significantly from their respected baselines (Figure 4).
2
Potassium, mmol/L 4.1 ± 0.2 4.2 ± 0.2 .341 Volumes of blood loss were the same between the control and
Ionized calcium, mmol/L 1.31 ± 0.06 1.34 ± 0.04 .16 AAJT-TP groups (3.3L ± 0.5L and 3.0L ± 0.5L, respectively;
pH 7.448 ± 0.039 7.457 ± 0.020 .52 p = .285). Both groups received the maximum amount of Hex-
Serum lactate, mmol/L 1.8 ± 0.6 2.2 ± 0.7 .198 tend allocated.
Hemoglobin, g/dL 10.6 ± 0.9 10.3 ± 0.7 .525 Fresh whole-blood administration during damage control sur-
Platelets 394 ± 80 339 ± 73 .094 gery did not differ between groups, nor did FFP administration
Injury characteristics during the ICU phase (Table 1). At the end of the prehospital
Transection, % 75.7 ± 8.0 80.9 ± 7.3 .114 period, there was no significant difference in heart rate, MAP,
Blood loss, mL 3,263 ± 542 3,038 ± 457 .285 cardiac output, or partial pressure of carbon dioxide between
Heart rate, bpm 113 ± 38 133 ± 34 .204 groups. MAP, lactate, hemoglobin, and platelet values differed
Systolic BP, mmHg 46 ± 17 41 ± 12 .394 from baseline for both groups. At the end of the study, there
MAP, mmHg 28 ± 11 27 ± 8 .744 was no significant difference between groups in any physio-
EtCO , mmHg 23 ± 11 18 ± 5 .145 logic parameters (Table 1).
2
End of prehospital care (60 minutes after injury)
All animals received 1,000 1,000 1 As shown in Figure 5, survival did not differ between the AA-
Hextend, mL JT-TP and control groups (p = .564). Upon necropsy, three
Damage control surgery of 12 swine in the AAJT-TP group and two of the 12 control
animals had thrombus in the inferior vena cava.
Fresh whole blood, mL 2,218 ± 650 2,667 ± 289 .303
Intensive care phase
Fresh frozen plasma, mL 400 ± 548 1,000 ± 250 .131 Discussion
Insulin/50% glucose, no. 0.6 ± 0.5 0.3 ± 0.6 .537 In this study, we investigated the modification of a junctional
Data given as mean ± SD unless otherwise indicated. tourniquet for use in the management of NCTH in the ab-
Abbreviations: AAJT-TP, Abdominal Aortic Junctional Tourniquet domen. The predicted advantages to this approach were sim-
modified with a prototype, accessory pressure distribution plate; BP, plicity of application and enhanced safety in comparison to
blood pressure; EtCO , end-tidal carbon dioxide; MAP, mean arterial
2
pressure; pCO , partial pressure of carbon dioxide, pO , partial pres- currently available technologies for NCTH, which are pri-
2
2
sure of oxygen; SvO , venous oxygen saturation. marily endovascular, requiring more training and resources.
2
108 | JSOM Volume 18, Edition 4 / Winter 2018