Page 29 - JSOM Summer 2018
P. 29
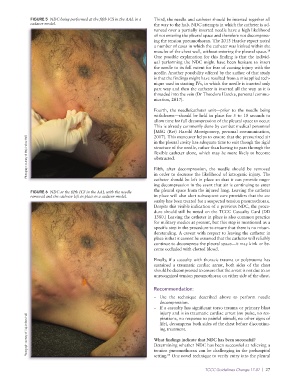
FIGURE 5 NDC being performed at the fifth ICS in the AAL in a Third, the needle and catheter should be inserted together all
cadaver model. the way to the hub. NDC attempts in which the catheter is ad-
vanced over a partially inserted needle have a high likelihood
of not entering the pleural space and therefore not decompress-
ing the tension pneumothorax. The 2013 Harcke report noted
a number of cases in which the catheter was kinked within the
muscles of the chest wall, without entering the pleural space.
18
One possible explanation for this finding is that the individ-
ual performing the NDC might have been hesitant to insert
the needle to its full extent for fear of causing injury with the
needle. Another possibility offered by the author of that study
is that the findings might have resulted from a misapplied tech-
nique used in starting IVs, in which the needle is inserted only
part way and then the catheter is inserted all the way as it is
threaded into the vein (Dr Theodore Harcke, personal commu-
nication, 2017).
Fourth, the needle/catheter unit—prior to the needle being
withdrawn—should be held in place for 5 to 10 seconds to
allow time for full decompression of the pleural space to occur.
This is already commonly done by combat medical personnel
[MSG (Ret) Harold Montgomery, personal communication,
2017). This maneuver helps to ensure that the pressurized air
Photograph courtesy of Maj Andrew Hall. structure of the needle, rather than having to pass through the
in the pleural cavity has adequate time to exit though the rigid
flexible catheter alone, which may be more likely to become
obstructed.
Fifth, after decompression, the needle should be removed
in order to decrease the likelihood of iatrogenic injury. The
catheter should be left in place so that it can provide ongo-
ing decompression in the event that air is continuing to enter
the pleural space from the injured lung. Leaving the catheter
FIGURE 6 NDC at the fifth ICS in the AAL with the needle
removed and the catheter left in place in a cadaver model. in place will also alert subsequent care providers that the ca-
sualty has been treated for a suspected tension pneumothorax.
De spite this visible indication of a previous NDC, the proce-
dure should still be noted on the TCCC Casualty Card (DD
1380.) Leaving the catheter in place is also common practice
for military medics at present, but this step is mentioned as a
specific step in the procedure to ensure that there is no misun-
derstanding. A caveat with respect to leaving the catheter in
place is that it cannot be assumed that the catheter will reliably
continue to decompress the pleural space—it may kink or be-
come occluded with clotted blood.
Finally, if a casualty with thoracic trauma or polytrauma has
sustained a traumatic cardiac arrest, both sides of the chest
should be decompressed to ensure that the arrest is not due to an
unrecognized tension pneumothorax on either side of the chest.
Recommendation:
– Use the technique described above to perform needle
decompression.
– If a casualty has significant torso trauma or primary blast
injury and is in traumatic cardiac arrest (no pulse, no res-
Photograph courtesy of Maj Andrew Hall. What findings indicate that NDC has been successful?
pirations, no response to painful stimuli, no other signs of
life), decompress both sides of the chest before discontinu-
ing treatment.
Determining whether NDC has been successful at relieving a
tension pneumothorax can be challenging in the prehospital
setting. One novel technique to verify entry into the pleural
83
TCCC Guidelines Change 17-02 | 27