Page 120 - JSOM Spring 2018
P. 120
be triggered by non-immunologic mechanisms. These include
physical factors, ethanol and some medications such as nar-
cotics (Table 1).
3
Food is the most common trigger for anaphylaxis from in-
fancy through young adulthood. Among adults, food allergies
are most likely to occur under the age of 30. While food al-
lergies can occur with any food, shellfish, tree nuts, fish, soy
and peanuts account for most cases. Cashews are an emerging
cause of anaphylaxis due to increasing consumption of this
nut. There are also reports of cross-reactivity between cashews
and pistachios. People who are stung by insects can become
sensitized to hymenoptera venom and develop large local reac-
tions to them. More than 5 percent of persons sensitized may
go on to later develop a systemic anaphylactic reaction (SAR).
Unfortunately, current testing methods cannot distinguish
among persons who undergo asymptomatic sensitization,
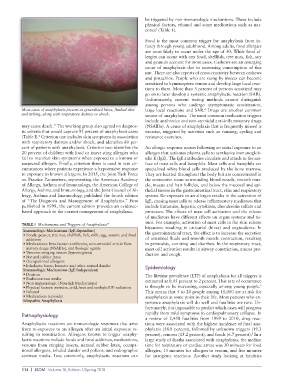
Most cases of anaphylaxis present as generalized hives, flushed skin large local reactions and SAR. Drugs are another common
4
and itching, along with respiratory distress or shock. source of anaphylaxis. The most common medication triggers
include antibiotics and non-steroidal anti-inflammatory drugs
may cause death.” The working group also agreed on diagnos- (NSAIDs). A cause of anaphylaxis that is frequently missed is
tic criteria that would capture 95 percent of anaphylaxis cases exercise, triggered by activities such as running, cycling and
(Table I). Criterion one includes skin symptoms in association resistance exercises.
2
with respiratory distress and/or shock, and identifies 80 per-
cent of patients with anaphylaxis. Criterion two identifies the An allergic response occurs following an initial exposure to an
20 percent of children with food or insect sting allergies who allergen that activates plasma cells to synthesize immunoglob-
fail to manifest skin symptoms when exposed to a known or ulin E (IgE). The IgE antibodies circulate and attach to the sur-
suspected allergen. Finally, criterion three is used in rare cir- face of mast cells and basophils. Mast cells and basophils are
cumstances where patients experience a hypotensive response specialized white blood cells produced by the bone marrow.
to exposure to known allergens. In 2015, the Joint Task Force They are located throughout the body but are concentrated in
on Practice Parameters, representing the American Academy the connective tissue surrounding blood vessels, smooth mus-
of Allergy, Asthma and Immunology, the American College of cle, mucus and hair follicles, and below the mucosal and epi-
Allergy, Asthma and Immunology, and the Joint Council of Al- thelial tissues in the gastrointestinal tract, skin and respiratory
lergy, Asthma and Immunology, published the fourth edition system. Re-exposure to an allergen results in the activation of
of “The Diagnosis and Management of Anaphylaxis.” First IgE, causing mast cells to release inflammatory mediators that
published in 1998, the current edition provides an evidence- include histamine, heparin, cytokines, chondroitin sulfate and
based approach to the current management of anaphylaxis. proteases. The effects of mast cell activation and the release
of mediators have different effects on organ systems and tis-
sues. For example, activation of mast cells in the skin release
TABLE I Mechanisms and Triggers of Anaphylaxis 17 histamine resulting in urticarial (hives) and angioedema. In
Immunologic Mechanisms (IgE dependent) the gastrointestinal tract, the effect is to increase the secretion
• Foods: peanut, tree nut, shellfish, fish, milk, egg, sesame and food
additives of intestinal fluids and smooth muscle contraction, resulting
• Medications: beta-lactam antibiotics, non-steroidal anti-inflam- in peristalsis, vomiting and diarrhea. In the respiratory tract,
matory drugs (NSAIDs), and biologic agents mast cell activation results in airway constriction, mucus pro-
• Venoms: stinging insects (hymenoptera) duction and cough.
• Natural rubber latex
• Occupational allergens
• Inhalants: horse, hamster and other animal dander Epidemiology
Immunologic Mechanisms (IgE Independent)
• Dextran The lifetime prevalence (LTP) of anaphylaxis for all triggers is
• Radiocontrast media estimated at 0.05 percent to 2 percent. This rate of occurrence
• Non-Immunologic (Non-IgE Mechanisms)
5
• Physical factors: exercise, cold, heat and sunlight/UV radiation is thought to be increasing, especially among young people.
• Ethanol This means that 5 to 20 people among 10,000 are at risk for
• Medications (opioids) anaphylaxis at some point in their life. Most patients who ex-
Idiopathic Anaphylaxis perience anaphylaxis will do well and fatalities are rare. Un-
fortunately, it is impossible to predict which cases will progress
rapidly from mild symptoms to cardiopulmonary collapse. In
Pathophysiology
a review of 2,458 fatalities from 1999 to 2010, drug reac-
Anaphylactic reactions are immunologic responses that arise tions were associated with the highest incidence of fatal ana-
from re-exposure to an allergen after an initial exposure re- phylaxis (58.8 percent), followed by unknown triggers (19.3
sulting in sensitization. Allergens known to trigger anaphy- percent), venoms (15.2 percent), and foods (6.7 percent). In a
6
lactic reactions include foods and food additives, medications, large study of deaths associated with anaphylaxis, the median
venoms from stinging insects, natural rubber latex, occupa- time for respiratory or cardiac arrest was 30 minutes for food
tional allergens, inhaled dander and pollens, and radiographic allergies, 15 minutes for allergies to venom, and five minutes
contrast media. Less commonly, anaphylactic reactions can for iatrogenic reactions. Another study looking at fatalities
114 | JSOM Volume 18, Edition 1/Spring 2018