Page 144 - Journal of Special Operations Medicine - Fall 2017
P. 144
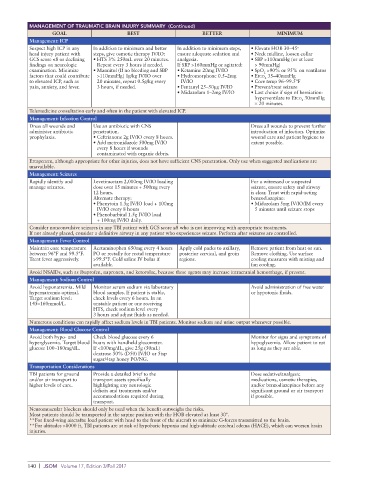
MANAGEMENT OF TRAUMATIC BRAIN INJURY SUMMARY (Continued)
GOAL BEST BETTER MINIMUM
Management: ICP
Suspect high ICP in any In addition to minimum and better In addition to minimum steps, • Elevate HOB 30–45 o
head injury patient with steps, give osmotic therapy IV/IO: ensure adequate sedation and • Neck midline, loosen collar
GCS score ≤8 or declining • HTS 3% 250mL over 20 minutes. analgesia. • SBP >110mmHg (or at least
findings on neurologic Repeat every 3 hours if needed. If SBP >160mmHg or agitated: > 90mmHg)
examination. Minimize • Mannitol (If no bleeding and SBP • Ketamine 20mg IV/IO • SpO >90% or 95% on ventilator
2
factors that could contribute >110mmHg) 1g/kg IV/IO over • Hydromorphone 0.5–2mg • Etco 35–40mmHg
2
to elevated ICP, such as 20 minutes, repeat 0.5g/kg every IV/IO • Core temp 96–99.5°F
pain, anxiety, and fever. 3 hours, if needed. • Fentanyl 25–50μg IV/IO • Prevent/treat seizure
• Midazolam 1–2mg IV/IO • Last choice if sign of herniation:
hyperventilate to Etco 30mmHg
2
× 20 minutes.
Telemedicine consultation early and often in the patient with elevated ICP.
Management: Infection Control
Dress all wounds and Use an antibiotic with CNS Dress all wounds to prevent further
administer antibiotic penetration. introduction of infection. Optimize
prophylaxis. • Ceftriaxone 2g IV/IO every 8 hours. wound care and patient hygiene to
• Add metronidazole 500mg IV/IO extent possible.
every 8 hours if wounds
contaminated with organic debris.
Ertapenem, although appropriate for other injuries, does not have sufficient CNS penetration. Only use when suggested medications are
unavailable.
Management: Seizures
Rapidly identify and Levetiracetam 2,000mg IV/IO loading For a witnessed or suspected
manage seizures. dose over 15 minutes + 500mg every seizure, ensure safety and airway
12 hours. is clear. Treat with rapid-acting
Alternate therapy: benzodiazepine:
• Phenytoin 1.5g IV/IO load + 100mg • Midazolam 5mg IV/IO/IM every
IV/IO every 8 hours 5 minutes until seizure stops
• Phenobarbital 1.5g IV/IO load
+ 100mg IV/IO daily.
Consider nonconvulsive seizures in any TBI patient with GCS score ≤8 who is not improving with appropriate treatments.
If not already placed, consider a definitive airway in any patient who experiences seizure. Perform after seizures are controlled.
Management: Fever Control
Maintain core temperature Acetaminophen 650mg every 4 hours Apply cold packs to axillary, Remove patient from heat or sun.
between 96°F and 99.5°F. PO or rectally for rectal temperature posterior cervical, and groin Remove clothing. Use surface
Treat fever aggressively. >99.5°F. Cold saline IV bolus if regions. cooling measures with misting and
available. fan cooling.
Avoid NSAIDs, such as ibuprofen, naproxen, and ketorolac, because these agents may increase intracranial hemorrhage, if present.
Management: Sodium Control
Avoid hyponatremia. Mild Monitor serum sodium via laboratory Avoid administration of free water
hypernatremia optimal. blood samples. If patient is stable, or hypotonic fluids.
Target sodium level: check levels every 6 hours. In an
145–160mmol/L. unstable patient or one receiving
HTS, check sodium level every
3 hours and adjust fluids as needed.
Numerous conditions can rapidly affect sodium levels in TBI patients. Monitor sodium and urine output whenever possible.
Management: Blood Glucose Control
Avoid both hypo- and Check blood glucose every 6 Monitor for signs and symptoms of
hyperglycemia. Target blood hours with handheld glucometer. hypoglycemia. Allow patient to eat
glucose 100–180mg/dL. If <100mg/dL, give 25g (50mL) as long as they are able.
dextrose 50% (D50) IV/IO or 5tsp
sugar/4tsp honey PO/NG.
Transportation Considerations
TBI patients for ground Provide a detailed brief to the Dose sedative/analgesic
and/or air transport to transport assets specifically medications, osmotic therapies,
higher levels of care. highlighting any neurologic and/or benzodiazepines before any
deficits and treatments and/or significant ground or air transport
accommodations required during if possible.
transport.
Neuromuscular blockers should only be used when the benefit outweighs the risks.
Most patients should be transported in the supine position with the HOB elevated at least 30°.
**For fixed-wing aircrafts: load patient with head to the front of the aircraft to minimize G-forces transmitted to the brain.
**For altitudes >8000 ft, TBI patients are at risk of hypobaric hypoxia and high-altitude cerebral edema (HACE), which can worsen brain
injuries.
140 | JSOM Volume 17, Edition 3/Fall 2017