Page 127 - Journal of Special Operations Medicine - Winter 2016
P. 127
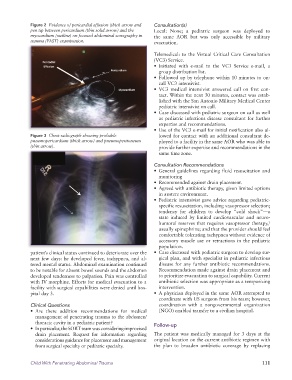
Figure 2 Evidence of pericardial effusion (thick arrow and Consultation(s)
pen tip between pericardium (thin solid arrow) and the Local: None; a pediatric surgeon was deployed to
myocardium (outline) on focused abdominal sonography in the same AOR but was only accessible by military
trauma (FAST) examination. evacuation.
Telemedical: to the Virtual Critical Care Consultation
(VC3) Service.
• Initiated with e-mail to the VC3 Service e-mail, a
group distribution list.
• Followed up by telephone within 10 minutes to on-
call VC3 intensivist.
• VC3 medical intensivist answered call on first con-
tact. Within the next 30 minutes, contact was estab-
lished with the San Antonio Military Medical Center
pediatric intensivist on call.
• Case discussed with pediatric surgeon on call as well
as pediatric infectious disease consultant for further
expertise and recommendations.
• Use of the VC3 e-mail for initial notification also al-
Figure 3 Chest radiograph showing probable lowed for contact with an additional consultant de-
pneumopericardium (thick arrow) and pneumoperitoneum ployed to a facility in the same AOR who was able to
(thin arrow). provide further expertise and recommendations in the
same time zone.
Consultation Recommendations
• General guidelines regarding fluid resuscitation and
monitoring
• Recommended against drain placement.
• Agreed with antibiotic therapy, given limited options
in austere environment.
• Pediatric intensivist gave advice regarding pediatric-
specific resuscitation, including vasopressor selection;
tendency for children to develop “cold shock”—a
state induced by limited cardiovascular and neuro-
1
humoral reserves that requires vasopressor therapy,
usually epinephrine; and that the provider should feel
comfortable tolerating tachypnea without evidence of
accessory muscle use or retractions in the pediatric
population.
patient’s clinical status continued to deteriorate over the • Case discussed with pediatric surgeon to develop sur-
next few days: he developed fever, tachypnea, and al- gical plan, and with specialist in pediatric infectious
tered mental status. Abdominal examination continued disease for any further antibiotic recommendations.
to be notable for absent bowel sounds and the abdomen Recommendation made against drain placement and
developed tenderness to palpation. Pain was controlled to prioritize evacuation to surgical capability. Current
with IV morphine. Efforts for medical evacuation to a antibiotic selection was appropriate as a temporizing
facility with surgical capabilities were denied until hos- intervention.
pital day 3. • A physician deployed in the same AOR attempted to
coordinate with US surgeon from his team; however,
Clinical Questions coordination with a nongovernmental organization
• Are there addition recommendations for medical (NGO) enabled transfer to a civilian hospital.
management of penetrating trauma to the abdomen/
thoracic cavity in a pediatric patient? Follow-up
• In particular, the SORT team was considering improvised
drain placement. Request for information regarding The patient was medically managed for 3 days at the
considerations guidance for placement and management original location on the current antibiotic regimen with
from surgical specialty or pediatric specialty. the plan to broaden antibiotic coverage by replacing
Child With Penetrating Abdominal Trauma 111