Page 98 - Journal of Special Operations Medicine - Summer 2016
P. 98
with patients. In addition, the use of zero, mild, mod- conditions as well as how they measure what constitutes
erate, and severe pain levels corresponding to the pain successful pain management.
intensity colors and bars was included to conform to
the 4-point pain scale used by the United Kingdom and Importantly, the DVPRS incorporates four supplemen-
other North Atlantic Treaty Organization (NATO) mili- tal questions with numeric ratings (0–10) that allow a
tary partners. 37 patient to identify how much his/her pain interferes with
physical activity and sleep and how it affects mood and
Perhaps the most important evolution on this new scale contributes to stress. All of these dimensions of pain
was the integration of functional language anchors assessment represent basic and important areas for im-
aimed at recasting the experience of pain in terms of proving our understanding of how pain influences a per-
functional disturbance as it relates to pain intensity. Fig- son’s life (Figure 2). These supplemental questions are
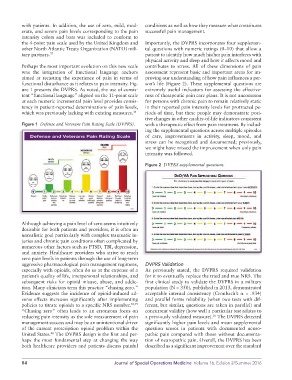
ure 1 presents the DVPRS. As noted, the use of consis- extremely useful indicators for assessing the effective-
tent “functional language” aligned on the 11-point scale ness of therapeutic pain care plans. It is not uncommon
at each numeric incremental pain level provides consis- for persons with chronic pain to remain relatively static
tency in patient-reported determinations of pain levels, in their reported pain intensity levels for protracted pe-
which was previously lacking with existing measures. 36 riods of time, but these people may demonstrate posi-
tive changes in other quality-of-life indicators consistent
Figure 1 Defense and Veterans Pain Rating Scale (DVPRS). with a therapeutic effect from pain treatment. By includ-
ing the supplemental questions across multiple episodes
of care, improvements in activity, sleep, mood, and
stress can be recognized and documented; previously,
we might have missed the improvement when only pain
intensity was followed.
Figure 2 DVPRS supplemental questions.
Although achieving a pain level of zero seems intuitively
desirable for both patients and providers, it is often an
unrealistic goal particularly with complex traumatic in-
juries and chronic pain conditions often complicated by
numerous other factors such as PTSD, TBI, depression,
and anxiety. Healthcare providers who strive to reach
zero pain levels in patients through the use of long-term
aggressive pharmacological pain management regimens, DVPRS Validation
especially with opioids, often do so at the expense of a As previously stated, the DVPRS required validation
patient’s quality of life, interpersonal relationships, and for it to eventually replace the tried and true NRS. The
subsequent risks for opioid misuse, abuse, and addic- first clinical study to validate the DVPRS in a military
tion. Many clinicians term this practice “chasing zero.” population (N = 350), published in 2013, demonstrated
Evidence suggests the incidence of opioid-induced ad- acceptable internal consistency (Cronbach’s α = .934)
verse effects increases significantly after implementing and parallel forms reliability (when two tests with dif-
policies to titrate opioids to a specific NRS number. 38,39 ferent, but similar, questions are taken in parallel) and
“Chasing zero” often leads to an erroneous focus on concurrent validity (how well a particular test relates to
reducing pain intensity as the sole measurement of pain a previously validated measure). The DVPRS detected
36
management success and may be an unintentional driver significantly higher pain levels and mean supplemental
of the current prescription opioid problem within the question scores in patients with documented neuro-
United States. The DVPRS design is the first and per- pathic pain compared with those without documenta-
40
haps the most fundamental step at changing the way tion of neuropathic pain. Overall, the DVPRS has been
both healthcare providers and patients discuss painful described as a significant improvement over the standard
84 Journal of Special Operations Medicine Volume 16, Edition 2/Summer 2016