Page 20 - JSOM Winter 2024
P. 20
hemorrhage by 50%. However, these interventions are un- anatomy lab records for the selected donors, as was photo-
likely to ever fall within the practice scope of combat med- graphic and scientific consent. Ethics board approval was not
ics. Resuscitative endovascular balloon occlusion of the aorta sought as this is not required for UK cadaver studies.
15
(REBOA) is an invasive means of arresting NCTH, but this
6,9
is not a combat medic–delivered intervention. The American A single pilot cadaver was used to test, re-test, validate, and
College of Surgeons Committee on Trauma and the American streamline the test process (This cadaver was pre-excluded
College of Emergency Physicians have also stated that REBOA from the research due to a prominent midline laparotomy
should only be employed by a trained acute surgeon, or by an scar). For each test cadaver, one 4-cm manometric water-filled
emergency physician or interventionalist when an acute care balloon was placed intraperitoneally in the epigastric space
surgeon is immediately available. A major recent randomized and another in the retropubic space by two consultant trauma
16
trial has shown that REBOA use increased bleeding and mor- surgeons. These were each connected to manometer tubing,
tality at all time points. A matched cohort trial on REBOA a syringe, and three-way tap (Figure 2). Skin around the out-
17
in pelvic trauma showed significantly increased mortality and lets was clipped to form a seal. Baseline pressures of 8cmH O
2
18
worse outcomes. We believe REBOA use may well now be were set (equating to mean human intra-abdominal pressure
29
significantly curtailed, if not discontinued. [IAP].) The AAJT-S was then applied correctly: abdominally,
centered on the umbilicus, and inflated to 250mmHg as per
The Abdominal Aortic Junctional Tourniquet – Stabilized manufacturer instructions for use. Steady pressure readings
( AAJT-S) (Compression Works Ltd, Birmingham, AL) is an ex- were then recorded for both compartments (Figure 3). The
ternally applied device that compresses the descending aorta AAJT-S was then deflated and removed, along with the epi-
in zone 3 (infrarenal) via a pneumatic bladder (Figure 1). It gastric manometer. Intra-abdominal hemorrhage was simu-
has been shown in animal and human cases 19,20 to be effec- lated by pouring 500mL of water into the abdominal cavity
tive at temporizing hemorrhage previously considered ‘non- via the epigastric aperture and allowed to distribute over at
compressible’ in zone 3 of the descending aorta, below the least 5 minutes (Figure 4). The epigastric manometer was re-
renal vessels. AAJT-S has also been shown to improve physi- placed, and again, IAPs of 8cmH O were reset. The AAJT-S
2
ological parameters in hemorrhage. 21,22 It has been repeatedly was then reapplied, centered on the umbilicus and inflated to
demonstrated that the AAJT-S has an aortic occlusion effect 250mmHg. Steady pressure readings were recorded for the
equivalent to zone 3 REBOA 22,23 as well as the ability to con- proximal epigastric and distal pelvic compartments.
vert an AAJT-S to a REBOA. 24,25 Non-physicians and Com-
bat Medical Technicians have been demonstrated to be able These steady IAPs were used in subsequent statistical analysis
to effectively apply AAJT-S to healthy humans in around 30 using a Microsoft Excel 365 Data Analysis.
seconds, following a brief training period. Human case series
26
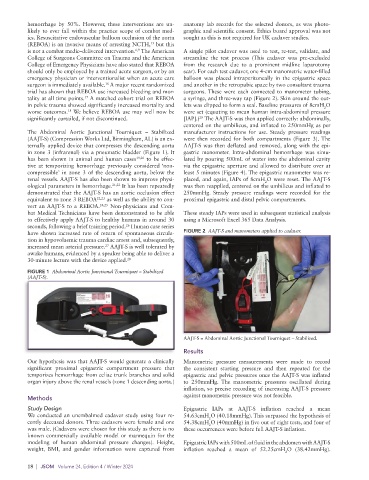
have shown increased rate of return of spontaneous circula- FIGURE 2 AAJT-S and manometers applied to cadaver.
tion in hypovolaemic trauma cardiac arrest and, subsequently,
increased mean arterial pressure. AAJT-S is well tolerated by
27
awake humans, evidenced by a speaker being able to deliver a
30-minute lecture with the device applied. 28
FIGURE 1 Abdominal Aortic Junctional Tourniquet – Stabilized
(AAJT-S).
AAJT-S = Abdominal Aortic Junctional Tourniquet – Stabilized.
Results
Our hypothesis was that AAJT-S would generate a clinically Manometric pressure measurements were made to record
significant proximal epigastric compartment pressure that the consistent starting pressure and then repeated for the
temporizes hemorrhage from celiac trunk branches and solid epigastric and pelvic pressures once the AAJT-S was inflated
organ injury above the renal vessels (zone 1 descending aorta.) to 250mmHg. The manometric pressures oscillated during
inflation, so precise recording of increasing AAJT-S pressure
against manometric pressure was not feasible.
Methods
Study Design Epigastric IAPs at AAJT-S inflation reached a mean
We conducted an unembalmed cadaver study using four re- 54.63cmH O (40.18mmHg). This surpassed the hypothesis of
2
cently deceased donors. Three cadavers were female and one 54.38cmH O (40mmHg) in five out of eight tests, and four of
2
was male. (Cadavers were chosen for this study as there is no these occurrences were before full AAJT-S inflation.
known commercially available model or mannequin for the
modeling of human abdominal pressure changes). Height, Epigastric IAPs with 500mL of fluid in the abdomen with AAJT-S
weight, BMI, and gender information were captured from inflation reached a mean of 52.25cmH O (38.42mmHg).
2
18 | JSOM Volume 24, Edition 4 / Winter 2024