Page 52 - JSOM Spring 2023
P. 52
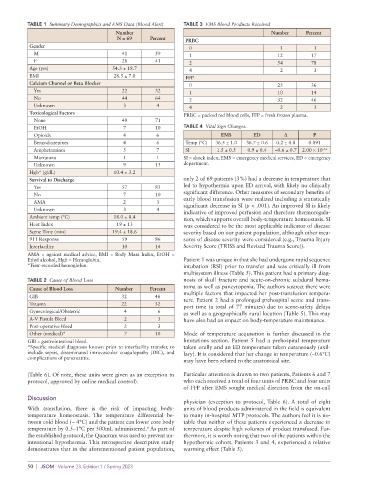
TABLE 1 Summary Demographics and EMS Data (Blood Alert) TABLE 3 EMS Blood Products Received
Number Number Percent
N = 69 Percent PRBC
Gender 0 1 1
M 41 59 1 12 17
F 28 41 2 54 78
Age (yrs) 54.3 ± 18.7 4 2 3
BMI 28.5 ± 7.0 FFP
Calcium Channel or Beta Blocker 0 25 36
Yes 22 32 1 10 14
No 44 64 2 32 46
Unknown 3 4 4 2 3
Toxicological Factors PRBC = packed red blood cells, FFP = fresh frozen plasma.
None 49 71
EtOH 7 10 TABLE 4 Vital Sign Changes.
Opioids 4 6 EMS ED Δ P
Benzodiazepines 4 6 Temp (°C) 36.5 ± 1.0 36.7 ± 0.6 0.2 ± 0.8 0.091
Amphetamines 5 7 SI 1.5 ± 0.5 0.9 ± 0.4 –0.6 ± 0.7 2.00 × 10 –16
Marijuana 1 1 SI = shock index, EMS = emergency medical services, ED = emergency
Unknown 9 13 department.
Hgb* (g/dL) 10.4 ± 3.2
Survival to Discharge only 2 of 69 patients (3%) had a decrease in temperature that
Yes 57 83 led to hypothermia upon ED arrival, with likely no clinically
No 7 10 significant difference. Other measures of secondary benefits of
early blood transfusion were realized including a statistically
AMA 2 3 significant decrease in SI (p < .001). An improved SI is likely
Unknown 3 4 indicative of improved perfusion and therefore thermoregula-
Ambient temp (°C) 18.0 ± 8.4 tion, which supports overall body-temperature homeostasis. SI
Heat Index 19 ± 13 was considered to be the most applicable indicator of disease
Scene Time (min) 19.4 ± 18.6 severity based on our patient population, although other mea-
911 Response 59 86 sures of disease severity were considered (e.g., Trauma Injury
Interfacility 10 14 Severity Score (TRISS and Revised Trauma Score)).
AMA = against medical advice, BMI = Body Mass Index, EtOH =
Ethyl alcohol, Hgb = Hemoglobin. Patient 1 was unique in that she had undergone rapid sequence
*First-recorded hemoglobin. intubation (RSI) prior to transfer and was critically ill from
multisystem illness (Table 5). This patient had a primary diag-
TABLE 2 Cause of Blood Loss nosis of skull fracture and acute-on-chronic subdural hema-
Cause of Blood Loss Number Percent toma as well as pancytopenia. The authors suspect there were
GIB 32 46 multiple factors that impacted her post-transfusion tempera-
ture. Patient 2 had a prolonged prehospital scene and trans-
Trauma 22 32 port time (a total of 77 minutes) due to scene-safety delays
Gynecological/Obstetric 4 6 as well as a geographically rural location (Table 5). This may
A-V Fistula Bleed 2 3 have also had an impact on body-temperature maintenance.
Post-operative Bleed 2 3
Other (medical)* 7 10 Mode of temperature acquisition is further discussed in the
GIB = gastrointestinal bleed. limitations section. Patient 5 had a prehospital temperature
*Specific medical diagnoses known prior to interfacility transfer, to taken orally and an ED temperature taken cutaneously (axil-
include sepsis, disseminated intravascular coagulopathy (DIC), and lary). It is considered that her change in temperature (–0.6°C)
complications of pancreatitis.
may have been related to the anatomical site.
(Table 6). Of note, these units were given as an exception to Particular attention is drawn to two patients, Patients 6 and 7
protocol, approved by online medical control). who each received a total of four units of PRBC and four units
of FFP after EMS sought medical direction from the on-call
Discussion
physician (exception to protocol, Table 6). A total of eight
With transfusion, there is the risk of impacting body- units of blood products administered in the field is equivalent
temperature homeostasis. The temperature differential be- to many in-hospital MTP protocols. The authors feel it is no-
tween cold blood (~ 4°C) and the patient can lower core body table that neither of these patients experienced a decrease in
temperature by 0.5–1°C per 500mL administered. As part of temperature despite high volumes of product transfused. Fur-
8
the established protocol, the Quantum was used to prevent un- thermore, it is worth noting that two of the patients within the
intentional hypothermia. This retrospective descriptive study hypothermic cohort. Patients 3 and 4, experienced a relative
demonstrates that in the aforementioned patient population, warming effect (Table 5).
50 | JSOM Volume 23, Edition 1 / Spring 2023