Page 112 - JSOM Spring 2023
P. 112
TABLE 3 Clinical Outcomes of Patients Divided between the Low, Moderate, and High % pFVC Groups with Statistical Comparison
Low Moderate High
FVC 0–29% FVC 30–49% FVC 50+%
(n = 23) (n = 36) (n = 20) P-value
Pneumonia, n (%) 0 (0) 0 (0) 0 (0) —
ARDS, n (%) 0 (0) 0 (0) 0 (0) —
Pulmonary Embolism, n (%) 0 (0) 0 (0) 0 (0) —
Retained Hemothorax, n (%) 1 (4.4) 0 (0) 0 (0) 0.291
Empyema, n (%) 0 (0) 0 (0) 0 (0) —
Aspiration Pneumonitis, n (%) 0 (0) 0 (0) 0 (0) —
Unplanned Intubation, n (%) 1 (4.4) 2 (5.6) 0 (0) .479
ICU Readmission, n (%) 2 (8.7) 2 (5.6) 0 (0) .198
Pulmonary Complications, n (%) 2 (8.7) 2 (5.6) 0 (0) .198
Hospital LOS, mean (SD) 7.26 (4.114) 7.31 (5.903) 4.15 (2.477) .043
ICU LOS, mean (SD) 3.35 (2.497) 3.28 (3.961) 1.90 (3.095) .215
Non-Home Discharge, n (%) 5 (21.7) 12 (33.3) 1 (5.6) .031
Readmission, n (%) 0 (0) 0 (0) 1 (5.0) —
Death, n (%) 0 (0) 1 (2.8) 0 (0) —
% pFVC = percent predicted forced vital capacity, ARDS = Acute Respiratory Distress Syndrome, ICU = intensive care unit, LOS = length of stay
number of total ribs fractured compared to those discharged the findings of increased hospital and ICU LOS and increased
home (mean = 7.722, standard deviation = 3.675 vs. mean = discharge to a non-home facility for patients with decreased %
5.967, standard deviation = 2.689, p = .036). pFVC on admission, the measure does correlate with increased
hospital and postdischarge care requirements.
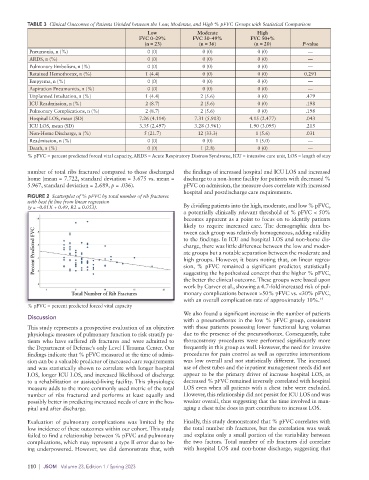
FIGURE 2 Scatterplot of % pFVC by total number of rib fractures
with best fit line from linear regression
(y = –0.01X + 0.49, R2 = 0.053). By dividing patients into the high, moderate, and low % pFVC,
a potentially clinically relevant threshold of % pFVC < 50%
becomes apparent as a point to focus on to identify patients
likely to require increased care. The demographic data be-
Percent Predicted FVC to the findings. In ICU and hospital LOS and non-home dis-
tween each group was relatively homogeneous, adding validity
charge, there was little difference between the low and moder-
ate groups but a notable separation between the moderate and
high groups. However, it bears noting that, on linear regres-
sion, % pFVC remained a significant predictor, statistically
suggesting the hypothesized concept that the higher % pFVC,
the better the clinical outcome. These groups were based upon
work by Carver et al., showing a 4.7-fold increased risk of pul-
Total Number of Rib Fractures monary complications between >50% pFVC vs. <30% pFVC,
with an overall complication rate of approximately 10%. 13
% pFVC = percent predicted forced vital capacity
We also found a significant increase in the number of patients
Discussion with a pneumothorax in the low % pFVC group, consistent
This study represents a prospective evaluation of an objective with these patients possessing lower functional lung volumes
physiologic measure of pulmonary function to risk stratify pa- due to the presence of the pneumothorax. Consequently, tube
tients who have suffered rib fractures and were admitted to thoracostomy procedures were performed significantly more
the Department of Defense’s only Level I Trauma Center. Our frequently in this group as well. However, the need for invasive
findings indicate that % pFVC measured at the time of admis- procedures for pain control as well as operative interventions
sion can be a valuable predictor of increased care requirements was low overall and not statistically different. The increased
and was statistically shown to correlate with longer hospital use of chest tubes and the inpatient management needs did not
LOS, longer ICU LOS, and increased likelihood of discharge appear to be the primary driver of increase hospital LOS, as
to a rehabilitation or assisted-living facility. This physiologic decreased % pFVC remained inversely correlated with hospital
measure adds to the more commonly used metric of the total LOS even when all patients with a chest tube were excluded.
number of ribs fractured and performs at least equally and However, this relationship did not persist for ICU LOS and was
possibly better in predicting increased needs of care in the hos- weaker overall, thus suggesting that the time involved in man-
pital and after discharge. aging a chest tube does in part contribute to increase LOS.
Evaluation of pulmonary complications was limited by the Finally, this study demonstrated that % pFVC correlates with
low incidence of these outcomes within our cohort. This study the total number rib fractures, but the correlation was weak
failed to find a relationship between % pFVC and pulmonary and explains only a small portion of the variability between
complications, which may represent a type II error due to be- the two factors. Total number of rib fractures did correlate
ing underpowered. However, we did demonstrate that, with with hospital LOS and non-home discharge, suggesting that
110 | JSOM Volume 23, Edition 1 / Spring 2023