Page 54 - JSOM Winter 2022
P. 54
combination as the participant when necessary to record ob- TABLE 2 Demographics of Consented Subjects
servations. Time was stopped when the participant inflated the n = 32
cuff of the airway and stated they were finished. The manne- Years as Corpsman (mean (SD)) 3.4 (3.3)
quin was then checked to ensure proper placement.
Prior Cricothyrotomy Experience 32
Between iterations, participants replaced their blackout gog- With TCK 19
gles, and the mannequin was reset, with intact silicone over the With BA 3
cricothyrotomy site. Participants were not given any feedback Unsure which kit 11
regarding their performance until completion of all four itera- Low Light Procedure Experience 17
tions. After completion of all four iterations, participants com- Training 15
pleted a post-event survey in which they rated their confidence In Field 3
and perceived degree of difficulty while using each light source.
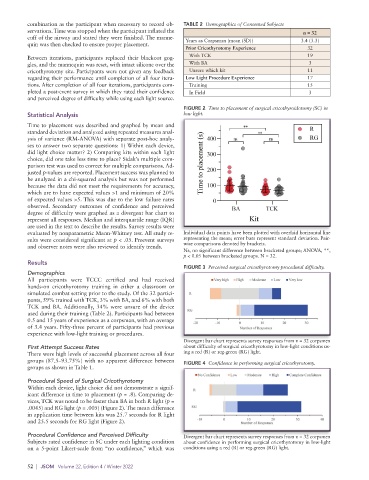
FIGURE 2 Time to placement of surgical cricothyroidotomy (SC) in
Statistical Analysis low light.
Time to placement was described and graphed by mean and
standard deviation and analyzed using repeated measures anal-
ysis of variance (RM-ANOVA) with separate post-hoc analy-
ses to answer two separate questions: 1) Within each device,
did light choice matter? 2) Comparing kits within each light
choice, did one take less time to place? Sidak’s multiple com-
parison test was used to correct for multiple comparisons. Ad-
justed p-values are reported. Placement success was planned to
be analyzed in a chi-squared analysis but was not performed
because the data did not meet the requirements for accuracy,
which are to have expected values >1 and minimum of 20%
of expected values >5. This was due to the low failure rates
observed. Secondary outcomes of confidence and perceived
degree of difficulty were graphed as a divergent bar chart to
represent all responses. Median and interquartile range (IQR)
are used in the text to describe the results. Survey results were
evaluated by nonparametric Mann-Whitney test. All study re- Individual data points have been plotted with overlaid horizontal line
sults were considered significant at p < .05. Preevent surveys representing the mean; error bars represent standard deviation. Pair-
and observer notes were also reviewed to identify trends. wise comparisons denoted by brackets.
Ns, no significant difference between bracketed groups; ANOVA, **,
p < 0.05 between bracketed groups. N = 32.
Results
FIGURE 3 Perceived surgical cricothyrotomy procedural difficulty.
Demographics
All participants were TCCC certified and had received
hands-on cricothyrotomy training in either a classroom or
simulated combat setting prior to the study. Of the 32 partici-
pants, 59% trained with TCK, 3% with BA, and 6% with both
TCK and BA. Additionally, 34% were unsure of the device
used during their training (Table 2). Participants had between
0.5 and 15 years of experience as a corpsman, with an average
of 3.4 years. Fifty-three percent of participants had previous
experience with low-light training or procedures.
Divergent bar chart represents survey responses from n = 32 corpsmen
First Attempt Success Rates about difficulty of surgical cricothyrotomy in low-light conditions us-
There were high levels of successful placement across all four ing a red (R) or reg-green (RG) light.
groups (87.5–93.75%) with no apparent difference between FIGURE 4 Confidence in performing surgical cricothyrotomy.
groups as shown in Table 1.
Procedural Speed of Surgical Cricothyrotomy
Within each device, light choice did not demonstrate a signif-
icant difference in time to placement (p = .8). Comparing de-
vices, TCK was noted to be faster than BA in both R light (p =
.0045) and RG light (p = .005) (Figure 2). The mean difference
in application time between kits was 25.7 seconds for R light
and 25.5 seconds for RG light (Figure 2).
Procedural Confidence and Perceived Difficulty Divergent bar chart represents survey responses from n = 32 corpsmen
Subjects rated confidence in SC under each lighting condition about confidence in performing surgical cricothyrotomy in low-light
on a 5-point Likert-scale from “no confidence,” which was conditions using a red (R) or reg-green (RG) light.
52 | JSOM Volume 22, Edition 4 / Winter 2022