Page 54 - JSOM Spring 2021
P. 54
TABLE 4 Success of Prehospital Needle Decompression Based on Indication
p Value
(vs hypoxia with
Indication Attempts Success % Outcome positive clinical exam)
Cardiopulmonary arrest alone 12 0 0.0 Achieved ROSC <.01
Cardiopulmonary arrest with positive 22 2 10.0 Achieved ROSC .06
clinical exam
Hemodynamic compromise 7 3 42.9 Improved hemodynamics .18
Hemodynamic compromise with positive
clinical exam 64 13 20.3 Improved hemodynamics <.01
Hypoxia alone 6 4 66.7 Improved hypoxia .63
Hypoxia with positive clinical exam 88 62 70.5 Improved hypoxia —
Improved vital signs and/or
Combined indications alone 5 3 60.0 .21
examination
Combined indications with positive 5 2 40.0 Improved vital signs and/or .12
clinical exam examination
Abnormal exam but no hemodynamic 124 65 52.4 Improved clinical <.01
impairment or hypoxia examination
ROSC = return of spontaneous circulation.
TABLE 5 Clinical Examination Ability to Augment Prehospital ND Success
Without Examination With Examination
Indication Success Attempts % Success Attempts % p Value
Cardiopulmonary arrest 0 12 0 2 22 9.1 .52
Hemodynamic compromise 3 7 42.9 13 64 20.3 .63
Hypoxia 4 6 66.7 62 88 70.5 .98
Combined Indications 3 5 60.0 2 5 40.0 .99
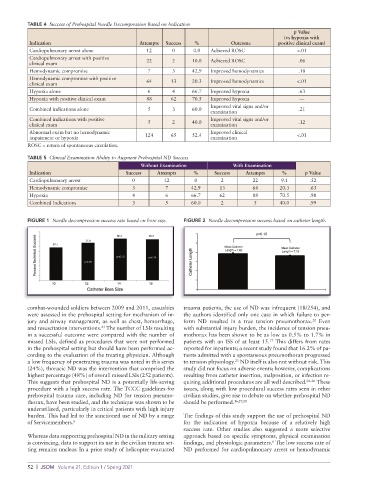
FIGURE 1 Needle decompression success rate based on bore size. FIGURE 2 Needle decompression success based on catheter length.
combat-wounded soldiers between 2009 and 2011, casualties trauma patients, the use of ND was infrequent (18/254), and
were assessed in the prehospital setting for mechanism of in- the authors identified only one case in which failure to per-
jury and airway management, as well as chest, hemorrhage, form ND resulted in a true tension pneumothorax. Even
22
and resuscitation interventions. The number of LSIs resulting with substantial injury burden, the incidence of tension pneu-
21
in a successful outcome were compared with the number of mothorax has been shown to be as low as 0.5% to 1.7% in
missed LSIs, defined as procedures that were not performed patients with an ISS of at least 15. This differs from rates
17
in the prehospital setting but should have been performed ac- reported for inpatients; a recent study found that 16.2% of pa-
cording to the evaluation of the treating physician. Although tients admitted with a spontaneous pneumothorax progressed
a low frequency of penetrating trauma was noted in this series to tension physiology. ND itself is also not without risk. This
23
(24%), thoracic ND was the intervention that comprised the study did not focus on adverse events; however, complications
highest percentage (48%) of overall missed LSIs (252 patients). resulting from catheter insertion, malposition, or infection re-
This suggests that prehospital ND is a potentially life-saving quiring additional procedures are all well described. 24–26 These
procedure with a high success rate. The TCCC guidelines for issues, along with low procedural success rates seen in other
prehospital trauma care, including ND for tension pneumo- civilian studies, give rise to debate on whether prehospital ND
thorax, have been studied, and the technique was shown to be should be performed. 16,27,28
underutilized, particularly in critical patients with high injury
burden. This had led to the sanctioned use of ND by a range The findings of this study support the use of prehospital ND
of Servicemembers. 8 for the indication of hypoxia because of a relatively high
success rate. Other studies also suggested a more selective
Whereas data supporting prehospital ND in the military setting approach based on specific symptoms, physical examination
is convincing, data to support its use in the civilian trauma set- findings, and physiologic parameters. The low success rate of
6
ting remains unclear. In a prior study of helicopter-evacuated ND performed for cardiopulmonary arrest or hemodynamic
52 | JSOM Volume 21, Edition 1 / Spring 2021