Page 53 - JSOM Spring 2021
P. 53
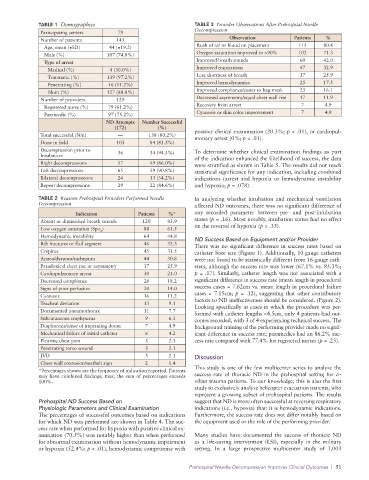
TABLE 1 Demographics TABLE 3 Provider Observations After Prehospital Needle
Decompression
Participating centers 79
Number of patients 143 Observation Patients %
Age, mean (±SD) 44 (±19.2) Rush of air or blood on placement 115 80.4
Male (%) 107 (74.8%) Oxygen saturation improved to >90% 102 71.3
Type of arrest Improved breath sounds 60 42.0
Medical (%) 4 (30.0%) Improved respirations 47 32.9
Traumatic (%) 139 (97.2%) Less shortness of breath 37 25.9
Penetrating (%) 16 (11.2%) Improved hemodynamics 25 17.5
Blunt (%) 127 (88.8%) Improved compliance/easier to bag-mask 23 16.1
Number of providers 129 Decreased asymmetry/equal chest wall rise 17 11.9
Registered nurse (%) 79 (61.2%) Recovery from arrest 7 4.9
Paramedic (%) 97 (75.2%) Cyanosis or skin color improvement 7 4.9
ND Attempts Number Successful
(172) (%)
Total successful (N/n) — 138 (80.2%) positive clinical examination (20.3%; p < .01), or cardiopul-
monary arrest (0%; p < .01).
Done in field 103 84 (81.5%)
Decompression prior to 36 34 (94.4%) To determine whether clinical examination findings as part
Intubation of the indication enhanced the likelihood of success, the data
Right decompressions 57 49 (86.0%) were stratified as shown in Table 5. The results did not reach
Left decompressions 65 59 (90.8%) statistical significance for any indication, including combined
Bilateral decompressions 24 13 (54.2%) indications (arrest and hypoxia or hemodynamic instability
Repeat decompressions 29 22 (84.6%) and hypoxia; p = .078).
TABLE 2 Reasons Prehospital Providers Performed Needle In analyzing whether intubation and mechanical ventilation
Decompression affected ND outcomes, there was no significant difference of
Indication Patients %* any recorded parameter between pre- and post-intubation
Absent or diminished breath sounds 120 83.9 states (p = .16). Most notably, intubation status had no effect
Low oxygen saturation (Spo ) 88 61.5 on the reversal of hypoxia (p = .35).
2
Hemodynamic instability 64 44.8 ND Success Based on Equipment and/or Provider
Rib fractures or flail segment 46 32.3 There was no significant difference in success rates based on
Crepitus 45 31.5 catheter bore size (Figure 1). Additionally, 10-gauge catheters
Apnea/dyspnea/tachypnea 44 30.8 were not found to be statistically different from 16-gauge cath-
Paradoxical chest rise or asymmetry 37 25.9 eters, although the success rate was lower (67.1% vs. 85.3%;
Cardiopulmonary arrest 30 21.0 p = .17). Similarly, catheter length was not associated with a
Decreased compliance 26 18.2 significant difference in success rate (mean length in procedural
Signs of poor perfusion 20 14.0 success cases = 7.62cm vs. mean length in procedural failure
Cyanosis 16 11.2 cases = 7.15cm; p = .12), suggesting that other contributory
factors to ND ineffectiveness should be considered. (Figure 2).
Tracheal deviation 13 9.1 Looking specifically at cases in which the procedure was per-
Documented pneumothorax 11 7.7 formed with catheter lengths <4.5cm, only 4 patients had out-
Subcutaneous emphysema 9 6.3 comes recorded, with 3 of 4 experiencing technical success. The
Diaphoresis/sense of impending doom 7 4.9 background training of the performing provider made no signif-
Mechanical failure of initial catheter 6 4.2 icant difference in success rate; paramedics had an 86.2% suc-
Pleuritic chest pain 3 2.1 cess rate compared with 77.4% for registered nurses (p = .23).
Penetrating torso wound 3 2.1
JVD 3 2.1 Discussion
Chest wall contusion/seatbelt sign 2 1.4
*Percentages shown are the frequency of indication reported. Patients This study is one of the few multicenter series to analyze the
may have combined findings; thus, the sum of percentages exceeds success rate of thoracic ND in the prehospital setting for ci-
100%. vilian trauma patients. To our knowledge, this is also the first
study to exclusively analyze helicopter evacuation patients, who
represent a growing subset of prehospital patients. The results
Prehospital ND Success Based on suggest that ND is more often successful at reversing respiratory
Physiologic Parameters and Clinical Examination indications (i.e., hypoxia) than it is hemodynamic indications.
The percentages of successful outcomes based on indications Furthermore, the success rate does not differ notably based on
for which ND was performed are shown in Table 4. The suc- the equipment used or the role of the performing provider.
cess rate when performed for hypoxia with positive clinical ex-
amination (70.5%) was notably higher than when performed Many studies have documented the success of thoracic ND
for abnormal examination without hemodynamic impairment as a life-saving intervention (LSI), especially in the military
or hypoxia (52.4%; p < .01), hemodynamic compromise with setting. In a large prospective multicenter study of 1,003
Prehospital Needle Decompression Improves Clinical Outcomes | 51