Page 107 - JSOM Spring 2021
P. 107
pressure was 90/40mmHg under 2mg/h norepinephrine infu- exposure of the wound was performed (Figure 2). Dissection
sion. His consciousness continued to deteriorate until he be- was carried down to superficial femoral vessels. There was a
came unresponsive, and his combined Glasgow Coma Scale large lateral laceration of the left superficial femoral artery and
score dropped to 6/15 (eyes, 1; verbal, 1; motor, 4). The left complete disruption with extremity lacerations of the left fem-
groin wound was still actively bleeding, so a second tourni- oral vein. For this exsanguinated patient, a damage-control
quet was applied. However, because the wound was located at procedure was decided on by agreement between the surgeon
the top of the thigh, the tourniquet was not effective, and the and the anesthetist. Primary repair by arteriorrhaphy with a
hemorrhage was not controlled. A junctional tourniquet was continuous suture line of 6-0 polypropylene was completed
therefore put in place (SAM Junctional Tourniquet [SAM-JT]; for the superficial femoral artery. Because of insufficient
SAM Medical) (Figure 1). Once the belt had been placed back-bleeding, two passages of Fogarty balloon catheters were
around the pelvis, the Target Compression Device was inflated undertaken. Venous injury was larger, and so simple ligation
with a hand pump until the bleeding stopped. The first hemo- of distal and proximal segments of the femoral vein was de-
globin level in point-of-care testing was 10.1g/dL. The massive cided on. Because of the short duration of the surgery and
transfusion protocol was activated; 2 type O, Rh-negative red the isolated injury, no fasciotomy was performed. Distal pulses
blood cell units and 2 lyophilized plasma units were immedi- were perceived with signs of revascularization at the end of
ately delivered and transfused to the patient. surgery.
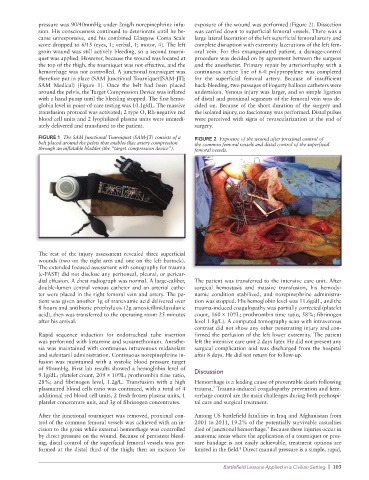
FIGURE 1 The SAM Junctional Tourniquet (SAM-JT) consists of a FIGURE 2 Exposure of the wound after proximal control of
belt placed around the pelvis that enables iliac artery compression the common femoral vessels and distal control of the superficial
through an inflatable bladder (the “target compression device”). femoral vessels.
The rest of the injury assessment revealed three superficial
wounds (two on the right arm and one on the left buttock).
The extended focused assessment with sonography for trauma
(e-FAST) did not disclose any peritoneal, pleural, or pericar-
dial effusion. A chest radiograph was normal. A large-caliber, The patient was transferred to the intensive care unit. After
double-lumen central venous catheter and an arterial cathe- surgical hemostasis and massive transfusion, his hemody-
ter were placed in the right femoral vein and artery. The pa- namic condition stabilized, and norepinephrine administra-
tient was given another 1g of tranexamic acid delivered over tion was stopped. His hemoglobin level was 11.6g/dL, and the
8 hours and antibiotic prophylaxis (2g amoxicillin/clavulanic trauma-induced coagulopathy was partially corrected (platelet
acid), then was transferred to the operating room 25 minutes count, 160 ´ 10 /L; prothrombin time ratio, 58%; fibrinogen
9
after his arrival. level 1.8g/L). A computed tomography scan with intravenous
contrast did not show any other penetrating injury and con-
Rapid sequence induction for endotracheal tube insertion firmed the perfusion of the left lower extremity. The patient
was performed with ketamine and suxamethonium. Anesthe- left the intensive care unit 2 days later. He did not present any
sia was maintained with continuous intravenous midazolam surgical complication and was discharged from the hospital
and sufentanil administration. Continuous norepinephrine in- after 8 days. He did not return for follow-up.
fusion was maintained with a systolic blood pressure target
of 90mmHg. First lab results showed a hemoglobin level of Discussion
9.1g/dL; platelet count, 209 ´ 10 /L; prothrombin time ratio,
9
28%; and fibrinogen level, 1.2g/L. Transfusion with a high Hemorrhage is a leading cause of preventable death following
plasma:red blood cells ratio was continued, with a total of 4 trauma. Trauma-induced coagulopathy prevention and hem-
7
additional red blood cell units, 2 fresh-frozen plasma units, 1 orrhage control are the main challenges during both prehospi-
platelet concentrate unit, and 3g of fibrinogen concentrates. tal care and surgical treatment.
After the junctional tourniquet was removed, proximal con- Among US battlefield fatalities in Iraq and Afghanistan from
trol of the common femoral vessels was achieved with an in- 2001 to 2011, 19.2% of the potentially survivable casualties
cision to the groin while external hemorrhage was controlled died of junctional hemorrhage. Because these injuries occur in
7
by direct pressure on the wound. Because of persistent bleed- anatomic areas where the application of a tourniquet or pres-
ing, distal control of the superficial femoral vessels was per- sure bandage is not easily achievable, treatment options are
formed at the distal third of the thigh; then an incision for limited in the field. Direct manual pressure is a simple, rapid,
8
Battlefield Lessons Applied in a Civilian Setting | 103