Page 102 - JSOM Spring 2021
P. 102
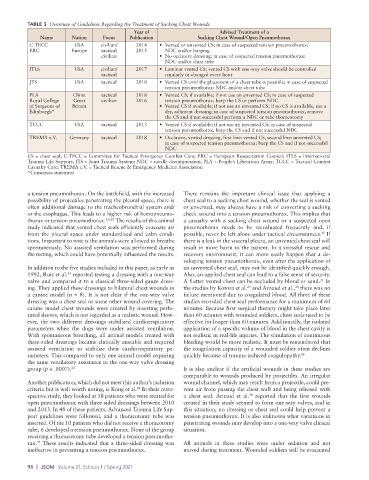
TABLE 3 Overview of Guidelines Regarding the Treatment of Sucking Chest Wounds
Year of Advised Treatment of a
Name Nation Focus Publication Sucking Chest Wound/Open Pneumothorax
C-TECC USA civilian/ 2014 • Vented or unvented CS; in case of suspected tension pneumothorax:
ERC Europe tactical 2015 NDC and/or burping
civilian • No occlusive dressing; in case of suspected tension pneumothorax:
NDC and/or chest tube
ITLS USA civilian/ 2017 • Laminar vented CS; vented CS with one-way valve should be controlled
tactical regularly or changed every hour
JTS USA tactical 2018 • Vented CS until the placement of a chest tube is possible; in case of suspected
tension pneumothorax: NDC and/or chest tube
PLA China tactical 2018 • Vented CS; if available; if not use an unvented CS; in case of suspected
Royal College Great civilian 2016 tension pneumothorax, burp the CS or perform NDC
of Surgeons of Britain • Vented CS if available; if not use an unvented CS; if no CS is available, use a
Edinburgh* dry, adherent dressing; in case of suspected tension pneumothorax, remove
the CS and if not successful perform a NDC or tube thoracotomy
TCCC USA tactical 2013 • Vented CS if available; if not use an unvented CS; in case of suspected
tension pneumothorax, burp the CS and if not successful NDC
TREMA e.V. Germany tactical 2018 • Occlusive, vented dressing, first line: vented CS, second line: unvented CS;
in case of suspected tension pneumothorax: burp the CS and if not successful
NDC
CS = chest seal; C-TECC = Committee for Tactical Emergency Combat Care; ERC = European Resuscitation Council; ITLS = International
Trauma Life Support; JTS = Joint Trauma System; NDC = needle decompression; PLA = People’s Liberation Army; TCCC = Tactical Combat
Casualty Care; TREMA e.V. = Tactical Rescue & Emergency Medicine Association
*Consensus statement
a tension pneumothorax. On the battlefield, with the increased There remains the important clinical issue that applying a
possibility of projectiles penetrating the pleural space, there is chest seal to a sucking chest wound, whether the seal is vented
often additional damage to the tracheobronchial system and/ or unvented, may always have a risk of converting a sucking
or the esophagus. This leads to a higher risk of hemopneumo- check wound into a tension pneumothorax. This implies that
thorax or tension pneumothorax. 5,6,24 The results of this animal a casualty with a sucking chest wound or a suspected open
study indicated that vented chest seals efficiently evacuate air pneumothorax needs to be reevaluated frequently and, if
from the pleural space under standardized and calm condi- possible, never be left alone under tactical circumstances. If
45
tions. Important to note is the animals were allowed to breathe there is a leak in the visceral pleura, an unvented chest seal will
spontaneously. No assisted ventilation was performed during result in more harm to the patient. In a stressful rescue and
the testing, which could have potentially influenced the results. recovery environment, it can more easily happen that a de-
veloping tension pneumothorax, even after the application of
In addition to the five studies included in this paper, as early as an unvented chest seal, may not be identified quickly enough.
1992, Ruiz et al. reported testing a dressing with a one-way Also, an applied chest seal can lead to a false sense of security.
43
valve and compared it to a classical three-sided gauze dress- A flutter vented chest can be occluded by blood or sand. In
31
ing. They applied these dressings to bilateral chest wounds in the studies by Kotora et al. and Arnaud et al., there was no
29
28
a canine model (n = 8). It is not clear if the one-way valve failure mentioned due to coagulated blood. All three of these
dressing was a chest seal or some other wound covering. The studies recorded chest seal performance for a maximum of 60
canine model chest wounds were created by inserting perfo- minutes. Because first surgical therapy might take place later
rated sleeves, which is not regarded as a realistic wound. How- than 60 minutes with wounded soldiers, chest seals need to be
ever, the two different dressings stabilized cardiorespiratory effective for longer than 60 minutes. Additionally, the isolated
parameters when the dogs were under assisted ventilation. application of a specific volume of blood in the chest cavity is
With spontaneous breathing, all animal models treated with not realistic in real-life injuries. The simulation of continuous
three-sided dressings became clinically unstable and required bleeding would be more realistic. It must be remembered that
assisted ventilation to stabilize their cardiorespiratory pa- the coagulation capacity of a wounded soldier often declines
rameters. This compared to only one animal model requiring quickly because of trauma-induced coagulopathy. 46
the same ventilatory assistance in the one-way valve dressing
group (p = .0007). 43 It is also unclear if the artificial wounds in these studies are
comparable to wounds produced by projectiles. An irregular
Another publication, which did not meet this author’s inclusion wound channel, which may result from a projectile, could pre-
criteria but is well worth noting, is Kong et al. In their retro- vent air from passing the chest wall and being released with
44
spective study, they looked at 58 patients who were treated for a chest seal. Arnaud et al. reported that the first wounds
28
open pneumothorax with three-sided dressings between 2010 created in their study seemed to form one-way valves, and in
and 2013. In 48 of these patients, Advanced Trauma Life Sup- this situation, no dressing or chest seal could help prevent a
port guidelines were followed, and a thoracotomy tube was tension pneumothorax. It is also unknown what variations in
inserted. Of the 10 patients who did not receive a thoracotomy penetrating wounds may develop into a one-way valve clinical
tube, 6 developed a tension pneumothorax. None of the group situation.
receiving a thoracotomy tube developed a tension pneumotho-
rax. These results indicated that a three-sided dressing was All animals in these studies were under sedation and not
44
ineffective in preventing a tension pneumothorax. moved during treatment. Wounded soldiers will be evacuated
98 | JSOM Volume 21, Edition 1 / Spring 2021