Page 39 - JSOM Spring 2020
P. 39
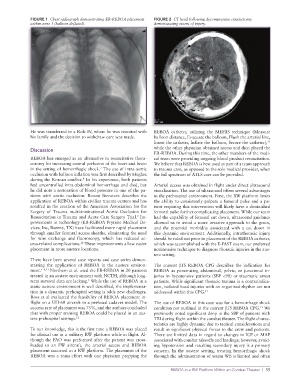
FIGURE 1 Chest radiograph demonstrating ER-REBOA placement FIGURE 2 CT head following decompressive craniectomy
within zone 1 (balloon deflated). demonstrating extent of injury.
He was transferred to a Role IV, where he was reunited with REBOA catheter, utilizing the MEFIIS technique (Measure
his family and the decision to withdraw care was made. balloon distance, Evacuate the balloon, Flush the arterial line,
Insert the catheter, Inflate the balloon, Secure the catheter),
13
Discussion while the other physician obtained access and then placed the
ER-REBOA. During this time, the other members of the medi-
REBOA has emerged as an alternative to resuscitative thora- cal team were providing ongoing blood product resuscitation.
cotomy for increasing central perfusion of the heart and brain We believe that REBOA is best used as part of a team approach
in the setting of hemorrhagic shock. The use of intra-aortic to trauma care, as opposed to the solo medical provider, when
7
occlusion with balloon inflation was first described by Hughes the full spectrum of ATLS care can be provided.
during the Korean conflict. In his experience, both patients
8
had uncontrolled intra-abdominal hemorrhage and died, but Arterial access was obtained in flight under direct ultrasound
he did note a restoration of blood pressure in one of the pa- visualization. The use of ultrasound offers several advantages
tients with aortic occlusion. Recent literature describes the in the prehospital environment. First, the RW platform limits
application of REBOA within civilian trauma centers and has the ability to consistently palpate a femoral pulse and a pa-
resulted in the creation of the American Association for the tient requiring this intervention will likely have a diminished
Surgery of Trauma multi-institutional Aortic Occlusion for femoral pulse further complicating placement. While our team
Resuscitation in Trauma and Acute Care Surgery Trial. Im- had the capability of femoral cut down, ultrasound guidance
9
provements in technology (ER-REBOA Prytime Medical De- allowed us to avoid a more invasive approach to the groin,
vices, Inc, Boerne, TX) have facilitated more rapid placement and the potential morbidity associated with a cut down in
through smaller femoral access sheaths, eliminating the need this dynamic environment. Additionally, intrathoracic injury
for wire exchange and fluoroscopy, which has reduced ac- should be ruled out prior to placement of the REBOA catheter,
cess-related complications. These improvements allow easier which was accomplished with the E-FAST exam, our preferred
10
placement in more austere locations. noninvasive technique to diagnose thoracic injuries in the aus-
tere setting.
There have been several case reports and case series demon-
strating the application of REBOA in the austere environ- The current JTS REBOA CPG describes the indication for
ment. 4–6,11 Northern et al. used the ER-REBOA in 20 patients REBOA as penetrating abdominal, pelvic, or junctional in-
treated in an austere environment with NCTH, although long- juries in hypotensive patients (SBP <90) or traumatic arrest
term survival data are lacking. While the use of REBOA in a patients. While significant thoracic trauma is a contraindica-
5
static austere environment is well described, the implementa- tion, isolated head injuries with an organized rhythm are not
tion in a dynamic prehospital setting is adds new challenges. addressed within this CPG. 13
Ross et al evaluated the feasibility of REBOA placement in-
flight on a UH-60 aircraft in a perfused cadaver model. The The use of REBOA in this case was for a hemorrhage shock
success rate of placement was 75%, and the authors concluded condition not outlined in the current JTS REBOA CPG. We
13
that with proper training REBOA could be placed in an aus- previously noted significant drop in the SBP of patients with
tere prehospital settings. 12 TBI during flight within the combat theater. The flight charac-
teristics are highly dynamic due to tactical considerations and
To our knowledge, this is the first time a REBOA was placed result in significant physical forces to the crew and patients.
for clinical use in a military RW platform while in flight. Al- There are limited data in regard to changes in ICP or MAP
though the PAO was performed after the patient was cross- associated with combat takeoffs and landings; however, avoid-
loaded to an FW aircraft, the arterial access and REBOA ing hypotension and resulting secondary injury is a primary
placement occurred in a RW platform. The placement of the concern. In the austere setting, treating hemorrhagic shock
REBOA was a team effort with one physician prepping the through the administration of warm WB is limited and often
REBOA in a RW Platform Within an Combat Theater | 35