Page 36 - JSOM Spring 2020
P. 36
patient became bradycardic, diaphoretic, and hypotensive. His 20mg IV or 0.1–0.2mg/kg IV for moderate pain. Importantly,
22
heart rate and blood pressure dropped to 37 and 79/48 (59), this is an identical dose given to our subject patient.
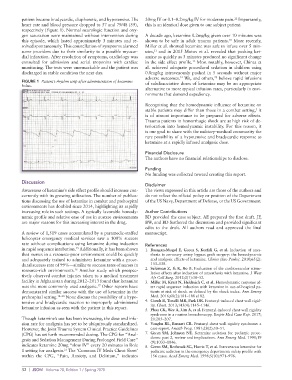
respectively (Figure 1). Normal neurologic function and oxy-
gen saturation were maintained without intervention during A decade ago, ketamine 0.2mg/kg given over 10 minutes was
this episode, which lasted approximately 3 minutes and re- shown to be safe in adult trauma patients. More recently,
10
solved spontaneously. This constellation of symptoms alarmed Miller et al. showed ketamine was safe to infuse over 5 min-
some providers due to their similarity to a possible myocar- utes, and in 2015 Motov et al. revealed that pushing ket-
11
dial infarction. After resolution of symptoms, cardiology was amine as quickly as 3 minutes produced no significant change
consulted for admission and serial troponins with cardiac in the side effect profile. Most notably, however, Chinta et
12
monitoring. The tests were unremarkable and the patient was al. achieved adequate procedural sedation in children using
discharged in stable condition the next day. 0.8mg/kg intravenously pushed in 5 seconds without major
adverse outcomes. We, and others, believe rapid infusions
23
14
FIGURE 1 Patient’s rhythm strip after administration of ketamine of subdissociative doses of ketamine may be an appropriate
bolus.
alternative to more typical infusion rates, particularly in envi-
ronments that demand expediency.
Recognizing that the hemodynamic influence of ketamine on
stable patients may differ than those in a combat setting, it
3
is of utmost importance to be prepared for adverse effects.
Trauma patients in hemorrhagic shock are at high risk of de-
terioration into hemodynamic instability. For this reason, it
is our goal to share with the military–medical community the
rare possibility of a hypotensive and bradycardic response to
ketamine at a rapidly infused analgesic dose.
Financial Disclosure
The authors have no financial relationships to disclose.
Funding
No funding was collected toward creating this report.
Discussion
Disclaimer
Awareness of ketamine’s side effect profile should increase con- The views expressed in this article are those of the authors and
currently with its growing utilization. The number of publica- do not reflect the official policy or position of the Department
tions discussing the use of ketamine in combat and prehospital of the US Navy, Department of Defense, or the US Government.
environments has doubled since 2014, highlighting its rapidly
increasing role in such settings. A typically favorable hemody- Author Contributions
namic profile and relative ease of use in austere environments BD provided the case subject. AE prepared the first draft. JF,
are major reasons for this increasing interest in the drug. BW, and BD furthered the discussion and provided significant
edits to the draft. All authors read and approved the final
A review of 1,519 cases accumulated by a paramedic-staffed manuscript.
helicopter emergency medical services saw a 100% success
rate without complications using ketamine during induction References
in rapid sequence intubation. Additionally, it has been shown 1. Basagan-Mogol E, Goren S, Korfali G, et al. Induction of anes-
15
that nurses in a resource-poor environment could be quickly thesia in coronary artery bypass graft surgery: the hemodynamic
and adequately trained to administer ketamine with a proce- and analgesic effects of ketamine. Clinics (Sao Paulo). 2010;65(2):
dural success rate of 99%—similar to success rates of nurses in 133–138.
resource-rich environments. Another study which prospec- 2. Suleiman Z, Ik K, Bo B. Evaluation of the cardiovascular stimu-
16
tively observed combat injuries taken to a medical treatment lation effects after induction of anaesthesia with ketamine. J West
Afr Coll Surg. 2012;2(1):38–52.
facility in Afghanistan during 2012–2013 found that ketamine 3. Miller M, Kruit N, Heldreich C, et al. Hemodynamic response af-
was the most commonly used analgesic. Other reports have ter rapid sequence induction with ketamine in out-of-hospital pa-
17
demonstrated similar success with the use of ketamine in the tients at risk of shock as defined by the shock index. Ann Emerg
prehospital setting. 18–20 None discuss the possibility of a hypo- Med. 2016;68(2):181–188 e182.
tensive and bradycardic reaction to improperly administered 4. Coruh B, Tonelli MR, Park DR. Fentanyl-induced chest wall rigid-
ity. Chest. 2013;143(4):1145–1146.
ketamine infusion as seen with the patient in this report. 5. Phua CK, Wee A, Lim A, et al. Fentanyl-induced chest wall rigidity
syndrome in a routine bronchoscopy. Respir Med Case Rep. 2017;
Though ketamine’s use has been increasing, the dose and infu- 20:205–207.
sion rate for analgesia has yet to be ubiquitously standardized. 6. Vaughn RL, Bennett CR. Fentanyl chest wall rigidity syndrome: a
However, the Joint Trauma System Clinical Practice Guidelines case report. Anesth Prog. 1981;28(2):50–51.
(CPG) has set forth recommended dosing. The CPG for “Anal- 7. Green SM, Johnson NE. Ketamine sedation for pediatric proce-
gesia and Sedation Management During Prolonged Field Care” dures: part 2, review and implications. Ann Emerg Med. 1990;19
(9):1033–1046.
indicates ketamine 20mg “slow IV” every 20 minutes in Role 8. Green SM, Rothrock SG, Harris T, et al. Intravenous ketamine for
1 setting for analgesia. The ‘Common IV Meds Cheat Sheet’ pediatric sedation in the emergency department: safety profile with
21
within the CPG, “Pain, Anxiety, and Delirium,” indicates 156 cases. Acad Emerg Med. 1998;5(10):971–976.
32 | JSOM Volume 20, Edition 1 / Spring 2020