Page 22 - JSOM Summer 2019
P. 22
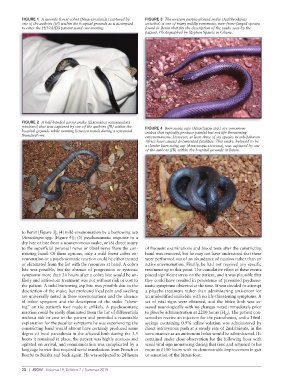
FIGURE 1 A juvenile forest cobra (Naja savannula) captured by FIGURE 3 The western purple-glossed snake (Amblyodipsas
one of the authors (JB) within the hospital grounds as it attempted unicolor) is one of many mildly venomous, non–front-fanged species
to enter the HIV/AIDS patient ward one evening. found in Benin that fits the description of the snake seen by the
patient. Photographed by Stephen Spawls in Ghana.
FIGURE 2 A half-banded garter snake (Elapsoidea semiannulata
moebiusi) that was captured by one of the authors (JB) within the FIGURE 4 Burrowing asps (Atractaspis spp.) are venomous
hospital grounds while running between wards during a torrential snakes that typically produce painful but not life-threatening
thunderstorm. envenomations. However, at least three of six species in sub-Saharan
Africa have caused documented fatalities. This snake, believed to be
a slender burrowing asp (Atractaspis aterrima), was captured by one
of the authors (JB) within the hospital grounds in Benin.
to Benin [Figure 3]; (4) mild envenomation by a burrowing asp
(Atractaspis spp. [Figure 4]); (5) psychosomatic response to a
dry bite or bite from a nonvenomous snake, or (6) direct injury
to the superficial peroneal nerve or tibial nerve from the con- of frequent examinations and blood tests after the constricting
stricting band. Of these options, only a mild forest cobra en- band was removed, but he may not have understood that these
venomation or a psychosomatic reaction could be either treated were performed out of an abundance of caution rather than an
or eliminated from the list with the resources at hand. A cobra active envenomation. Finally, he had not received any specific
bite was possible, but the absence of progression or systemic treatment up to this point. The cumulative effect of these events
symptoms more than 24 hours after a cobra bite would be un- placed significant stress on the patient, and it was plausible that
likely and antivenom treatment was not without risk or cost to they could have resulted in persistence of presumed psychoso-
the patient. A mild burrowing asp bite was possible due to the matic symptoms observed at the time. It was decided to attempt
description of the snake, but profound local pain and swelling a placebo treatment rather than administering antivenom for
are universally noted in these envenomations and the absence an unidentified snakebite with no life-threatening symptoms. A
of either symptom and the description of the snake “chew- set of vital signs were obtained, and the bitten limb was as-
ing” on the patient’s foot made it unlikely. A psychosomatic sessed neurologically with no changes noted immediately prior
reaction could be easily eliminated from the list of differentials to placebo administration at 2200 hours (H ). The patient con-
24
without risk or cost to the patient and provided a reasonable sented to receive an injection for the paresthesias, and a 10mL
explanation for the peculiar symptoms he was experiencing: the syringe containing 0.9% saline solution was administered by
constricting band would almost have certainly produced some direct intravenous push at a steady rate of 2mL/minute, in the
degree of local paresthesia in the affected limb during the 3.5 same manner as an antivenom bolus would be administered. He
hours it remained in place, the patient was highly anxious and remained under close observation for the following hour with
agitated on arrival, and communication was complicated by a serial vital sign monitoring during that time and returned to his
language barrier that required serial translations from French to room at 0100 hours with no demonstrable improvement in gait
Beerba to Bariba and back again. He was subjected to 24 hours or sensation of the bitten foot.
20 | JSOM Volume 19, Edition 2 / Summer 2019