Page 44 - JSOM Winter 2018
P. 44
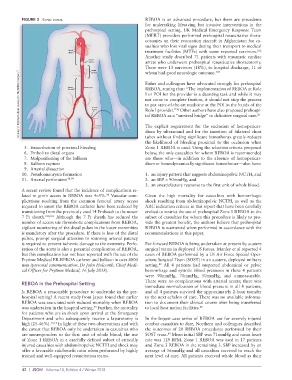
FIGURE 3 Aortic zones. REBOA is an advanced procedure, but there are precedents
for undertaking lifesaving but invasive interventions in the
prehospital setting. UK Medical Emergency Response Team
(MERT) providers performed prehospital resuscitative thora-
cotomies on their evacuation aircraft in Afghanistan for ca-
sualties who lost vital signs during their transport to medical
treatment facilities (MTFs) with some reported survivors.
102
Another study described 71 patients with traumatic cardiac
arrest who underwent prehospital resuscitative thoracotomy.
There were 13 survivors (18%), to hospital discharge, 11 of
Courtesy of Prytime Medical Devices, Inc. The REBOA Company ™ . REBOA, stating that: “The implementation of REBOA at Role
whom had good neurologic outcome.
103
Fisher and colleagues have advocated strongly for prehospital
I or POI for the provider is a daunting task and while it may
not come to complete fruition, it should not stop the process
to put state-of-the-art medicine at the POI in the hands of the
Role I provider.” Other authors have also proposed prehospi-
96
tal REBOA as a “survival bridge” to definitive surgical care.
26
The explicit requirement for the exclusion of hemopericar-
dium by ultrasound and for the insertion of bilateral chest
tubes without finding significant hemothorax greatly reduces
the likelihood of bleeding proximal to the occlusion when
5. Exacerbation of proximal bleeding Zone 1 REBOA is used. Using the selection criteria proposed
6. Emboli to distal organs below, the only casualties for whom REBOA is recommended
7. Malpositioning of the balloon are those who—in addition to the absence of hemopericar-
8. Balloon rupture dium or hemodynamically significant hemothorax—also have:
9. Arterial dissection
10. Pseudoaneurysm formation 1. an injury pattern that suggests abdominopelvic NCTH, and
11. Arterial perforation 98,99 2. an SBP < 90mmHg, and
3. an unsatisfactory response to the first unit of whole blood.
A recent review found that the incidence of complications re-
lated to groin access in REBOA was 4–5%. Vascular com- Given the high mortality for casualties with hemorrhagic
98
plications resulting from the common femoral artery access shock resulting from abdominopelvic NCTH, as well as the
required to insert the REBOA catheter have been reduced by ARC indication criteria in this report that have been carefully
transitioning from the previously used 14 Fr sheath to the newer crafted to restrict the use of prehospital Zone 1 REBOA to the
7 Fr sheath. 100,101 Although the 7 Fr sheath has reduced the subset of casualties for whom this procedure is likely to pro-
number of access site thrombotic complications from REBOA, vide the greatest benefit, the authors believe that prehospital
vigilant monitoring of the distal pulses in the lower extremities REBOA is warranted when performed in accordance with the
is mandatory after the procedure. If there is loss of the distal recommendations in this paper.
pulses, prompt surgical attention to restoring arterial patency
is required to prevent ischemic damage to the extremity. Perfo- Far-forward REBOA is being undertaken at present by austere
ration of the aorta is also a potential complication of REBOA, surgical teams in deployed US forces. Manley et al reported 4
but this complication has not been reported with the use of the cases of REBOA performed by a US Air Force Special Oper-
Prytime Medical ER-REBOA catheter and balloon in over 4000 ations Surgical Team (SOST) in an austere, deployed military
88
uses (personal communication, Dr John Holcomb, Chief Medi- setting. All 4 patients had suspected abdominal or pelvic
cal Officer for Prytime Medical, 16 July 2018). hemorrhage and systolic blood pressures in these 4 patients
were 90mmHg, 70mmHg, 50mmHg, and unmeasurable.
There were no complications with arterial access; there was
REBOA in the Prehospital Setting
immediate normalization of blood pressure in all 4 patients;
Is REBOA a reasonable procedure to undertake in the pre- and all 4 patients survived the approximately 2-hour transfer
hospital setting? A recent study from Japan found that earlier to the next echelon of care. There was no available informa-
REBOA was associated with reduced mortality when REBOA tion to document their clinical course after being transferred
was undertaken in the hospital setting. Further, the mortality to local host nation facilities. 88
95
for patients who are in shock upon arrival at the Emergency
Department and who subsequently receive a laparotomy is In the largest case series of REBOA use for severely injured
high (25-46%). 13,14 In light of these two observations and with combat casualties to date, Northern and colleagues described
the caveat that REBOA only be undertaken in casualties who the outcomes of 20 REBOA procedures performed by their
are nonresponders to the first unit of whole blood, the use SOST team. Mean initial SBP was 71mmHg and mean heart
84
of Zone 1 REBOA in a carefully defined subset of critically rate was 129 BPM. Zone 1 REBOA was used in 17 patients
injured casualties with abdominopelvic NCTH and shock may and Zone 3 REBOA in the remaining 3. SBP increased by an
offer a favorable risk/benefit ratio when performed by highly average of 56mmHg and all casualties survived to reach the
trained and well-equipped resuscitation teams. next level of care. All patients received whole blood as their
42 | JSOM Volume 18, Edition 4 / Winter 2018