Page 82 - JSOM Spring 2018
P. 82
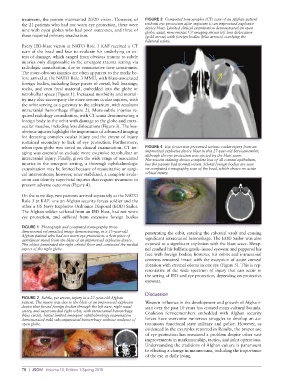
treatment, the patient maintained 20/20 vision. However, of FIGURE 3 Computed tomography (CT) scan of an Afghan patient
the 21 patients who had not worn eye protection, there were without eye protection after exposure to an improvised explosive
nine with open globes who had poor outcomes, and three of device blast. Limited clinical examination demonstrated an open
these required primary enucleation. globe; axial, noncontrast CT imaging shows left lens dislocation
(gold arrow) with foreign bodies (blue arrows) overlying the
bilateral sclera.
Every IED-blast victim at NATO Role 3 KAF received a CT
scan of the head and face to evaluate for underlying or ex-
tent of damage, which ranged from obvious trauma to subtle
injuries only diagnosable in the emergent trauma setting via
radiologic consultation, due to resuscitative time constraints.
The more-obvious injuries are often apparent to the medic be-
fore arrival at the NATO Role 3 MMU, with blast-associated
foreign bodies, including large pieces of metal, ball bearings,
rocks, and even fecal material, embedded into the globe or
retrobulbar space (Figure 1). Increased morbidity and mortal-
ity may also accompany the more serious ocular injuries, with
the orbit serving as a gateway to the calvarium, with resultant
intracranial hemorrhage (Figure 2). More-subtle injuries re-
quired radiology consultation, with CT scans demonstrating a
foreign body in the orbit with damage to the globe and extra-
ocular muscles, including lens dislocations (Figure 3). The less-
obvious injuries highlight the importance of advanced imaging
for detecting complex ocular injury and the extent of injury
sustained secondary to lack of eye protection. Furthermore,
when open globe was noted on clinical examination, CT im- FIGURE 4 Eye protection prevented serious ocular injury from an
aging was essential to exclude more extensive retrobulbar or improvised explosive device blast in this 27-year-old Servicemember,
intracranial injury. Finally, given the wide range of associated although the eye protection was ejected by the blast wave.
Fluorescein staining shows complete loss of all corneal epithelium,
injuries in the emergent setting, a thorough ophthalmologic but the patient had normal vision. Scleral foreign bodies are seen
examination may be limited because of resuscitative or surgi- on computed tomography scan of the head, which shows no acute
cal interventions; however, once stabilized, a complete evalu- orbital injury.
ation can identify superficial injuries that require treatment to
prevent adverse outcomes (Figure 4).
On the same day, two patients arrived separately at the NATO
Role 3 at KAF: one an Afghan security forces soldier and the
other a US Navy Explosive Ordnance Disposal (EOD) Sailor.
The Afghan soldier suffered from an IED blast, had not worn
eye protection, and suffered from extensive foreign bodies
FIGURE 1 Photograph and computed tomography three-
dimensional reformatted image demonstrating, in a 35-year-old penetrating the orbit, entering the calvarial vault and causing
Afghan patient who had not worn eye protection, a 4cm piece of significant intracranial hemorrhage. The EOD Sailor was also
curvilinear metal from the blast of an improvised explosive device.
The object penetrated the right orbital floor and contacted the medial exposed to a significant explosion with the blast wave. Shrap-
aspect of the right globe. nel crushed his ballistic-grade–issued eyewear and peppered his
face with foreign bodies; however, his orbits and intracranial
contents remained intact with the exception of acute corneal
abrasion with stromal edema in one eye (Figure 5). This is rep-
resentative of the wide spectrum of injury that can occur in
the setting of IED and eye protection, depending on protective
eyewear.
Discussion
FIGURE 2 Subtle, yet severe, injury in a 27-year-old Afghan
patient. The injury was due to the blast of an improvised explosive Western influence in the development and growth of Afghani-
device that forced foreign bodies through the left nare, right nasal stan over the past 10 years has crossed many cultural bounds.
cavity, and superomedial right orbit, with intracranial hemorrhage Coalition Servicemembers embedded with Afghan security
(blue circle). Initial limited emergent ophthalmology examination
demonstrated mild subconjunctival hemorrhage without evidence of forces have overcome numerous struggles to develop an au-
open globe. tonomous functional state military and police. However, as
evidenced in the examples reported in Results, the proper use
of eye protection has remained a problem despite other vast
improvements in marksmanship, tactics, and joint operations.
Understanding the traditions of Afghan culture is paramount
to effecting a change in mannerisms, including the importance
of the eye in daily living.
78 | JSOM Volume 18, Edition 1/Spring 2018