Page 132 - Journal of Special Operations Medicine - Fall 2017
P. 132
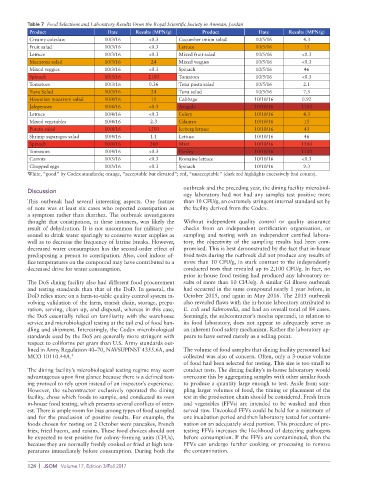
Table 7 Food Selections and Laboratory Results From the Royal Scientific Society in Amman, Jordan
Product Date Results (MPN/g) Product Date Results (MPN/g)
Creamy coleslaw 10/3/16 <0.3 Cucumber onion salad 10/5/16 4.3
Fruit salad 10/3/16 <0.3 Lettuce 10/5/16 15
Lettuce 10/3/16 <0.3 Mixed fruit salad 10/5/16 <0.3
Macaroni salad 10/3/16 24 Mixed veggies 10/5/16 <0.3
Mixed veggies 10/3/16 <0.3 Spinach 10/5/16 46
Spinach 10/3/16 2100 Tomatoes 10/5/16 <0.3
Tomatoes 10/3/16 0.36 Tuna pasta salad 10/5/16 2.1
Tuna Salad 10/3/16 24 Tuna salad 10/5/16 7.5
Hawaiian macaroni salad 10/4/16 15 Cabbage 10/10/16 0.92
Jalepenoes 10/4/16 <0.3 Arugula 10/10/16 1100
Lettuce 10/4/16 <0.3 Celery 10/10/16 4.3
Mixed vegetables 10/4/16 2.3 Cilantro 10/10/16 15
Potato salad 10/4/16 1500 Iceberg lettuce 10/10/16 43
Shrimp asparagus salad 10/4/16 1.1 Lettuce 10/10/16 46
Spinach 10/4/16 240 Mint 10/10/16 1500
Tomatoes 10/4/16 <0.3 Parsley 10/10/16 1100
Carrots 10/5/16 <0.3 Romaine lettuce 10/10/16 <0.3
Chopped eggs 10/5/16 <0.3 Spinach 10/10/16 9.3
White, “good” by Codex standards; orange, “acceptable but elevated”; red, “unacceptable” (dark red highlights excessively bad counts).
outbreak and the preceding year, the dining facility microbiol-
Discussion
ogy laboratory had not had any samples test positive more
This outbreak had several interesting aspects. One feature than 10 CFU/g, an extremely stringent internal standard set by
of note was at least six cases who reported constipation as the facility derived from the Codex.
a symptom rather than diarrhea. The outbreak investigators
thought that constipation, in these instances, was likely the Without independent quality control or quality assurance
result of dehydration. It is not uncommon for military per- checks from an independent certification organization, or
sonnel to drink water sparingly to conserve water supplies as sampling and testing with an independent certified labora-
well as to decrease the frequency of latrine breaks. However, tory, the objectivity of the sampling results had been com-
decreased water consumption has the second-order effect of promised. This is best demonstrated by the fact that in-house
predisposing a person to constipation. Also, cool indoor of- food tests during the outbreak did not produce any results of
fice temperatures on the compound may have contributed to a more than 10 CFU/g, in stark contrast to the independently
decreased drive for water consumption. conducted tests that revealed up to 2,100 CFU/g. In fact, no
prior in-house food testing had produced any laboratory re-
The DoS dining facility also had different food procurement sults of more than 10 CFUs/g. A similar GI illness outbreak
and testing standards than that of the DoD. In general, the had occurred in the same compound nearly 1 year before, in
DoD relies more on a farm-to-table quality control system in- October 2015, and again in May 2016. The 2015 outbreak
volving validation of the farm, transit chain, storage, prepa- also revealed flaws with the in-house laboratory attributed to
ration, serving, clean up, and disposal, whereas in this case, E. coli and Salmonella, and had an overall total of 84 cases.
the DoS essentially relied on familiarity with the warehouse Seemingly, the subcontractor’s modus operandi, in relation to
service and microbiological testing at the tail end of food han- its food laboratory, does not appear to adequately serve as
dling and shipment. Interestingly, the Codex microbiological an inherent food safety mechanism. Rather the laboratory ap-
standards used by the DoS are generally more stringent with pears to have served merely as a selling point.
respect to coliforms per gram than U.S. Army standards out-
lined in Army Regulation 40–70, NAVSUPINST 4355.6A, and The volume of food samples that dining facility personnel had
MCO 10110.44A. 3 collected was also of concern. Often, only a 3-ounce volume
of food had been selected for testing. This size is too small to
The dining facility’s microbiological testing regime may seem conduct tests. The dining facility’s in-house laboratory would
advantageous upon first glance because there is a defined test- overcome this by aggregating samples with other similar foods
ing protocol to rely upon instead of an inspector’s experience. to produce a quantity large enough to test. Aside from sam-
However, the subcontractor exclusively operated the dining pling larger volumes of food, the timing or placement of the
facility, chose which foods to sample, and conducted its own test in the production chain should be considered. Fresh fruits
in-house food testing, which presents several conflicts of inter- and vegetables (FFVs) are intended to be washed and then
est. There is ample room for bias among types of food sampled served raw. Uncooked FFVs could be held for a minimum of
and for the preclusion of positive results. For example, the one incubation period and then laboratory tested for contami-
foods chosen for testing on 2 October were pancakes, French nation on an adequately sized portion. This procedure of pre-
fries, fried bacon, and raisins. These food choices should not testing FFVs increases the likelihood of detecting pathogens
be expected to test positive for colony-forming units (CFUs), before consumption. If the FFVs are contaminated, then the
because they are normally freshly cooked or fried at high tem- FFVs can undergo further cooking or processing to remove
peratures immediately before consumption. During both the the contamination.
128 | JSOM Volume 17, Edition 3/Fall 2017