Page 49 - JSOM Spring 2026
P. 49
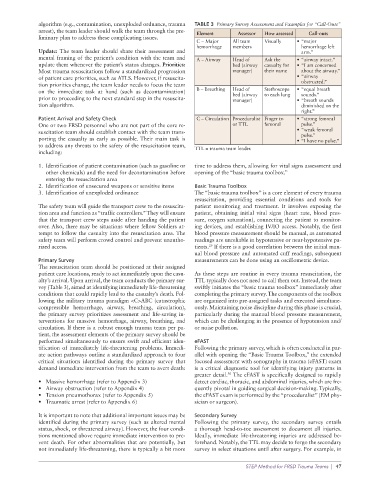
algorithm (e.g., contamination, unexploded ordnance, trauma TABLE 3 Primary Survey Assessment and Examples for “Call-Outs”
arrest), the team leader should walk the team through the pre- Element Assessor How assessed Call-outs
liminary plan to address these complicating issues.
C – Major All team Visually • “major
hemorrhage members hemorrhage left
Update: The team leader should share their assessment and arm.”
mental framing of the patient’s condition with the team and A – Airway Head of Ask the • “airway intact.”
update them whenever the patient’s status changes. Priorities: bed (airway casualty for • “I am concerned
Most trauma resuscitations follow a standardized progression manager) their name about the airway.”
of patient care priorities, such as ATLS. However, if resuscita- • “airway
tion priorities change, the team leader needs to focus the team obstructed.”
on the immediate task at hand (such as decontamination) B – Breathing Head of Stethoscope • “equal breath
sounds.”
prior to proceeding to the next standard step in the resuscita- bed (airway to each lung • “breath sounds
manager)
tion algorithm. diminished on the
right.”
Patient Arrival and Safety Check C – Circulation Proceduralist Finger to • “strong femoral
One or two FRSD personnel who are not part of the core re- or TTL femoral pulse.”
suscitation team should establish contact with the team trans- • “weak femoral
pulse.”
porting the casualty as early as possible. Their main task is • “I have no pulse.”
to address any threats to the safety of the resuscitation team, TTL = trauma team leader.
including:
1. Identification of patient contamination (such as gasoline or time to address them, allowing for vital signs assessment and
other chemicals) and the need for decontamination before opening of the “basic trauma toolbox.”
entering the resuscitation area
2. Identification of unsecured weapons or sensitive items Basic Trauma Toolbox
3. Identification of unexploded ordinance The “basic trauma toolbox” is a core element of every trauma
resuscitation, providing essential conditions and tools for
The safety team will guide the transport crew to the resuscita- patient monitoring and treatment. It involves exposing the
tion area and function as “traffic controllers.” They will ensure patient, obtaining initial vital signs (heart rate, blood pres-
that the transport crew steps aside after handing the patient sure, oxygen saturation), connecting the patient to monitor-
over. Also, there may be situations where fellow Soldiers at- ing devices, and establishing IV/IO access. Notably, the first
tempt to follow the casualty into the resuscitation area. The blood pressure measurement should be manual, as automated
safety team will perform crowd control and prevent unautho- readings are unreliable in hypotensive or near-hypotensive pa-
29
rized access. tients. If there is a good correlation between the initial man-
ual blood pressure and automated cuff readings, subsequent
Primary Survey measurements can be done using an oscillometric device.
The resuscitation team should be positioned at their assigned
patient care locations, ready to act immediately upon the casu- As these steps are routine in every trauma resuscitation, the
alty’s arrival. Upon arrival, the team conducts the primary sur- TTL typically does not need to call them out. Instead, the team
vey (Table 3), aimed at identifying immediately life-threatening swiftly initiates the “basic trauma toolbox” immediately after
conditions that could rapidly lead to the casualty’s death. Fol- completing the primary survey. The components of the toolbox
lowing the military trauma paradigm <C>ABC (catastrophic are organized into pre-assigned tasks and executed simultane-
compressible hemorrhage, airway, breathing, circulation), ously. Maintaining noise discipline during this phase is crucial,
the primary survey prioritizes assessment and life-saving in- particularly during the manual blood pressure measurement,
terventions for massive hemorrhage, airway, breathing, and which can be challenging in the presence of hypotension and/
circulation. If there is a robust enough trauma team per pa- or noise pollution.
tient, the assessment elements of the primary survey should be
performed simultaneously to ensure swift and efficient iden- eFAST
tification of immediately life-threatening problems. Immedi- Following the primary survey, which is often conducted in par-
ate action pathways outline a standardized approach to four allel with opening the “Basic Trauma Toolbox,” the extended
critical situations identified during the primary survey that focused assessment with sonography in trauma (eFAST) exam
demand immediate intervention from the team to avert death: is a critical diagnostic tool for identifying injury patterns in
greater detail. The eFAST is specifically designed to rapidly
30
• Massive hemorrhage (refer to Appendix 3) detect cardiac, thoracic, and abdominal injuries, which are fre-
• Airway obstruction (refer to Appendix 4) quently pivotal in guiding surgical decision-making. Typically,
• Tension pneumothorax (refer to Appendix 5) the eFAST exam is performed by the “proceduralist” (EM phy-
• Traumatic arrest (refer to Appendix 6) sician or surgeon).
It is important to note that additional important issues may be Secondary Survey
identified during the primary survey (such as altered mental Following the primary survey, the secondary survey entails
status, shock, or threatened airway). However, the four condi- a thorough head-to-toe assessment to document all injuries.
tions mentioned above require immediate intervention to pre- Ideally, immediate life-threatening injuries are addressed be-
vent death. For other abnormalities that are potentially, but forehand. Notably, the TTL may decide to forgo the secondary
not immediately life-threatening, there is typically a bit more survey in select situations until after surgery. For example, in
STEP Method for FRSD Trauma Teams | 47