Page 89 - Journal of Special Operations Medicine - Winter 2014
P. 89
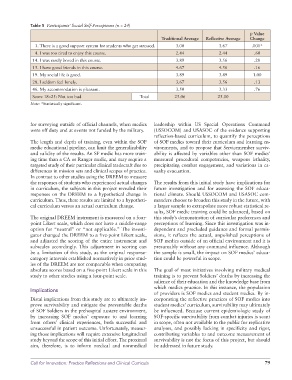
Table 5 Participants’ Social Self-Perceptions (n = 24)
p Value
Traditional Average Reflective Average Change
3. There is a good support system for students who get stressed. 3.00 3.67 .001*
4. I was too tired to enjoy this course. 2.44 2.44 .60
14. I was rarely bored in this course. 3.89 3.56 .28
15. I have good friends in this course. 4.67 4.56 .16
19. My social life is good. 3.89 3.89 1.00
28. I seldom feel lonely. 3.67 3.56 .13
46. My accommodation is pleasant. 3.50 3.33 .76
Score 18–25: Not too bad Total 25.06 25.00
Note: *Statistically significant.
for surveying outside of official channels, when medics leadership within US Special Operations Command
were off duty and at events not funded by the military. (USSOCOM) and USASOC of the evidence supporting
reflection-based curriculum, to quantify the perceptions
The length and depth of training, even within the SOF of SOF medics toward their curriculum and learning en-
medic educational pipeline, can limit the generalizability vironments, and to propose that Servicemember surviv-
and validity of the results. An SF medic has more train- ability is affected by variables other than SOF medics’
ing time than a CA or Ranger medic, and may require a measured procedural competencies, weapons lethality,
targeted study of their particular clinical tradecraft due to precipitating combat engagement, and variations in ca-
differences in mission sets and clinical scopes of practice. sualty evacuation.
In contrast to other studies using the DREEM to measure
the responses of students who experienced actual changes The results from this initial study have implications for
in curriculum, the subjects in this project revealed their future investigation and for assessing the SOF educa-
responses on the DREEM to a hypothetical change in tional climate. Should USSOCOM and USASOC com-
curriculum. Thus, these results are limited to a hypotheti- manders choose to broaden this study in the future, with
cal curriculum versus an actual curriculum change. a larger sample to extrapolate more robust statistical re-
sults, SOF medic training could be advanced, based on
The original DREEM instrument is measured on a four- this study’s demonstration of curricular preferences and
point Likert scale, which does not have a middle-range perceptions of learning. Since this investigation was in-
option for “neutral” or “not applicable.” The investi- dependent and precluded guidance and formal permis-
gator changed the DREEM to a five-point Likert scale, sions, it reflects the actual, unpolished perceptions of
and adjusted the scoring of the entire instrument and SOF medics outside of an official environment and it is
subscales accordingly. This adjustment in scoring can presumably without any command influence. Although
be a limitation of this study, as the original response- the sample is small, the impact on SOF medics’ educa-
category intervals established normatively in prior stud- tion could be powerful in scope.
ies of the DREEM are not comparable when comparing
absolute scores based on a five-point Likert scale in this The goal of most initiatives involving military medical
study to other studies using a four-point scale. training is to prevent Soldiers’ deaths by increasing the
salience of their education and the knowledge base from
which medics practice. In this instance, the population
Implications
of providers is SOF medics and student medics. By in-
Distal implications from this study are to ultimately im- corporating the reflective practices of SOF medics into
prove survivability and mitigate the preventable deaths student medics’ curriculum, survivability may ultimately
of SOF Soldiers in the prehospital austere environment, be influenced. Because current epidemiologic study of
by increasing SOF medics’ exposure to and learning SOF-specific survivability from combat injuries is scant
from others’ clinical experiences, both successful and in scope, often not available to the public for replicative
un successful in patient outcome. Unfortunately, measur- analyses, and possibly lacking in specificity and rigor,
ing those implications will require extensive longitudinal contributing variables to and outcome measurement of
study beyond the scope of this initial effort. The proximal survivability is not the focus of this project, but should
aim, therefore, is to inform medical and nonmedical be addressed in future study.
Call for Innovation: Practice Reflections and Clinical Curricula 79