Page 87 - Journal of Special Operations Medicine - Winter 2014
P. 87
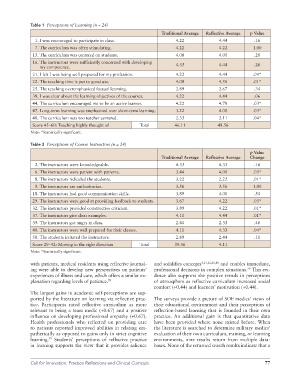
Table 1 Perceptions of Learning (n = 24)
Traditional Average Reflective Average p Value
1. I was encouraged to participate in class. 4.22 4.44 .16
7. The curriculum was often stimulating. 4.22 4.22 1.00
13. The curriculum was centered on students. 4.00 4.00 .28
16. The instructors were sufficiently concerned with developing 4.33 4.44 .26
my competence.
21. I felt I was being well prepared for my profession. 4.22 4.44 .04*
22. The teaching time is put to good use. 4.00 4.56 .01*
25. The teaching overemphasized factual learning. 2.89 2.67 .34
38. I was clear about the learning objectives of the courses. 4.22 4.44 .06
44. The curriculum encouraged me to be an active learner. 4.22 4.78 .03*
47. Long-term learning was emphasized over short-term learning. 3.22 4.00 .03*
48. The curriculum was too teacher centered. 2.33 2.11 .04*
Score 45–60: Teaching highly thought of Total 46.11 48.56
Note: *Statistically significant.
Table 2 Perceptions of Course Instructors (n = 24)
p Value
Traditional Average Reflective Average Change
2. The instructors were knowledgeable. 4.33 4.33 .16
6. The instructors were patient with patients. 3.44 4.00 .03*
8. The instructors ridiculed the students. 3.22 2.22 .01*
9. The instructors are authoritarian. 3.56 3.56 1.00
18. The instructors had good communication skills. 3.89 4.00 .54
29. The instructors were good at providing feedback to students. 3.67 4.22 .03*
32. The instructors provided constructive criticism. 3.89 4.22 .01*
37. The instructors give clear examples. 4.11 4.44 .01*
39. The instructors got angry in class. 2.44 2.33 .46
40. The instructors were well prepared for their classes. 4.11 4.33 .04*
50. The students irritated the instructors. 2.89 2.44 .11
Score 29–42: Moving in the right direction Total 39.56 4.11
Note: *Statistically significant.
with patients, medical residents using reflective journal- and solidifies concepts 9,21,22,26,80 and enables immediate,
ing were able to develop new perspectives on patients’ professional decisions in complex situations. This evi-
79
experiences of illness and care, which offers a similar ex- dence also supports the positive trends in perceptions
planation regarding levels of patience. 78 of atmosphere as reflective curriculum increased social
comfort (+0.44) and learners’ motivation (+0.44).
The largest gains in academic self-perceptions are sup-
ported by the literature on learning via reflective prac- The surveys provide a picture of SOF medics’ views of
tice. Participants rated reflective curriculum as more their educational environment and their perceptions of
relevant to being a team medic (+0.67) and a positive reflection-based learning that is founded in their own
influence on developing professional empathy (+0.67). practice. An additional gain is that quantitative data
Health professionals who reflected on providing care have been provided where none existed before. When
to patients reported improved abilities in relating em- the literature is searched to determine military medics’
pathetically as opposed to gains only in strict cognitive evaluation of their own curriculum, training, or learning
learning. Students’ perceptions of reflective practice environments, nine results return from multiple data-
79
in learning supports the view that it provides salience bases. None of the returned search results indicate that a
Call for Innovation: Practice Reflections and Clinical Curricula 77