Page 101 - 2022 Ranger Medic Handbook
P. 101
Medical Patient Assessment
Documentation of all healthcare provided is inherent with any form of care provided by Ranger Medical personnel.
Ranger Medics will document any and all assessments, healthcare, treatments, or procedures as appropriate to the
situation and setting. In the nontactical situation, healthcare will be documented on an SF 600, AHLTA electronic note or
trauma run sheet. In the tactical situation, care will be documented on the Ranger Casualty Card, DA5767 (TCCC Card),
or may be maintained in a notebook until subsequent annotation to the appropriate format. Referral to, communication
with, or review by a primary provider is required for all patients and notes.
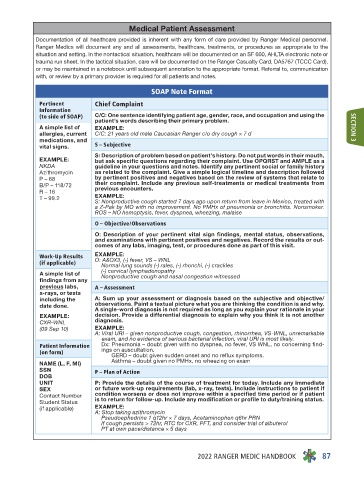
SOAP Note Format
Pertinent Chief Complaint
Information
(to side of SOAP) C/C: One sentence identifying patient age, gender, race, and occupation and using the
patient’s words describing their primary problem.
A simple list of EXAMPLE: SECTION 3
allergies, current C/C: 21 years old male Caucasian Ranger c/o dry cough × 7 d
medications, and
vital signs. S – Subjective
S: Description of problem based on patient’s history. Do not put words in their mouth,
EXAMPLE: but ask specific questions regarding their complaint. Use OPQRST and AMPLE as a
NKDA guideline in your questions and notes. Identify any pertinent social or family history
Azithromycin as related to the complaint. Give a simple logical timeline and description followed
P – 68 by pertinent positives and negatives based on the review of systems that relate to
B/P – 118/72 their complaint. Include any previous self-treatments or medical treatments from
previous encounters.
R – 16
T – 99.2 EXAMPLE:
S: Nonproductive cough started 7 days ago upon return from leave in Mexico, treated with
a Z-Pak by MO with no improvement. No PMHx of pneumonia or bronchitis. Nonsmoker.
ROS – NO hemoptysis, fever, dyspnea, wheezing, malaise
O – Objective/Observations
O: Description of your pertinent vital sign findings, mental status, observations,
and examinations with pertinent positives and negatives. Record the results or out-
comes of any labs, imaging, test, or procedures done as part of this visit.
Work-Up Results EXAMPLE:
(if applicable) O: A&OX3, (-) fever, VS – WNL
Normal lung sounds (-) rales, (-) rhonchi, (-) crackles
A simple list of (-) cervical lymphadenopathy
Nonproductive cough and nasal congestion witnessed
findings from any
previous labs, A – Assessment
x-rays, or tests
including the A: Sum up your assessment or diagnosis based on the subjective and objective/
date done. observations. Paint a textual picture what you are thinking the condition is and why.
A single-word diagnosis is not required as long as you explain your rationale in your
EXAMPLE: decision. Provide a differential diagnosis to explain why you think it is not another
CXR-WNL diagnosis.
(09 Sep 10) EXAMPLE:
A: Viral URI – given nonproductive cough, congestion, rhinorrhea, VS-WNL, unremarkable
exam, and no evidence of serious bacterial infection, viral URI is most likely.
Patient Information Dx: Pneumonia – doubt given with no dyspnea, no fever, VS WNL, no concerning find-
(on form) ings on auscultation.
GERD – doubt given sudden onset and no reflux symptoms.
NAME (L, F, MI) Asthma – doubt given no PMHx, no wheezing on exam
SSN P – Plan of Action
DOB
UNIT P: Provide the details of the course of treatment for today. Include any immediate
SEX or future work-up requirements (lab, x-ray, tests). Include instructions to patient if
Contact Number condition worsens or does not improve within a specified time period or if patient
Student Status is to return for follow-up. Include any modification or profile to duty/training status.
(if applicable) EXAMPLE:
A: Stop taking azithromycin
Pseudoephedrine 1 q12hr × 7 days, Acetaminophen q6hr PRN
If cough persists > 72hr, RTC for CXR, PFT, and consider trial of albuterol
PT at own pace/distance × 5 days
2022 RANGER MEDIC HANDBOOK 87