Page 79 - JSOM Summer 2022
P. 79
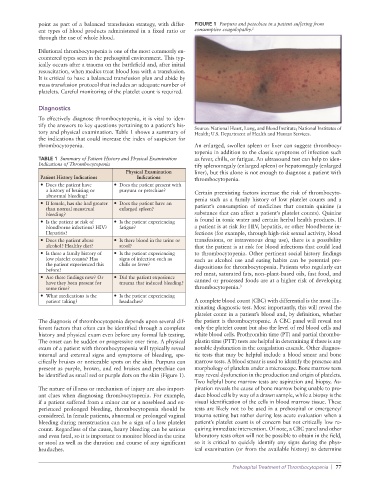
point as part of a balanced transfusion strategy, with differ- FIGURE 1 Purpura and petechiae in a patient suffering from
ent types of blood products administered in a fixed ratio or consumptive coagulopathy. 2
through the use of whole blood.
Dilutional thrombocytopenia is one of the most commonly en-
countered types seen in the prehospital environment. This typ-
ically occurs after a trauma on the battlefield and, after initial
resuscitation, when medics treat blood loss with a transfusion.
It is critical to have a balanced transfusion plan and abide by
mass transfusion protocol that includes an adequate number of
platelets. Careful monitoring of the platelet count is required.
Diagnostics
To effectively diagnose thrombocytopenia, it is vital to iden-
tify the answers to key questions pertaining to a patient’s his- Source: National Heart, Lung, and Blood Institute; National Institutes of
tory and physical examination. Table 1 shows a summary of Health; U.S. Department of Health and Human Services.
the indications that could increase the index of suspicion for
thrombocytopenia. An enlarged, swollen spleen or liver can suggest thrombocy-
topenia in addition to the classic symptoms of infection such
TABLE 1 Summary of Patient History and Physical Examination as fever, chills, or fatigue. An ultrasound test can help to iden-
Indications of Thrombocytopenia tify splenomegaly (enlarged spleen) or hepatomegaly (enlarged
Physical Examination liver), but this alone is not enough to diagnose a patient with
Patient History Indications Indications thrombocytopenia.
• Does the patient have • Does the patient present with
a history of bruising or purpura or petechiae? Certain preexisting factors increase the risk of thrombocyto-
abnormal bleeding? penia such as a family history of low platelet counts and a
• If female, has she had greater • Does the patient have an patient’s consumption of medicines that contain quinine (a
than normal menstrual enlarged spleen?
bleeding? substance that can affect a patient’s platelet counts). Quinine
• Is the patient at risk of • Is the patient experiencing is found in tonic water and certain herbal health products. If
bloodborne infections? HIV? fatigue? a patient is at risk for HIV, hepatitis, or other bloodborne in-
Hepatitis? fections (for example, through high-risk sexual activity, blood
• Does the patient abuse • Is there blood in the urine or transfusions, or intravenous drug use), there is a possibility
alcohol? Healthy diet? stool? that the patient is at risk for blood infections that could lead
• Is there a family history of • Is the patient experiencing to thrombocytopenia. Other pertinent social history findings
low platelet counts? Has signs of infection such as such as alcohol use and eating habits can be potential pre-
the patient experienced this chills or fever? dispositions for thrombocytopenia. Patients who regularly eat
before?
• Are these findings new? Or • Did the patient experience red meat, saturated fats, non–plant-based oils, fast food, and
have they been present for trauma that induced bleeding? canned or processed foods are at a higher risk of developing
some time? thrombocytopenia. 3
• What medications is the • Is the patient experiencing
patient taking? headaches? A complete blood count (CBC) with differential is the most illu-
minating diagnostic test. Most importantly, this will reveal the
platelet count in a patient’s blood and, by definition, whether
The diagnosis of thrombocytopenia depends upon several dif- the patient is thrombocytopenic. A CBC panel will reveal not
ferent factors that often can be identified through a complete only the platelet count but also the level of red blood cells and
history and physical exam even before any formal lab testing. white blood cells. Prothrombin time (PT) and partial thrombo-
The onset can be sudden or progressive over time. A physical plastin time (PTT) tests are helpful in determining if there is any
exam of a patient with thrombocytopenia will typically reveal notable dysfunction in the coagulation cascade. Other diagnos-
internal and external signs and symptoms of bleeding, spe- tic tests that may be helpful include a blood smear and bone
cifically bruises or noticeable spots on the skin. Purpura can marrow tests. A blood smear is used to identify the presence and
present as purple, brown, and red bruises and petechiae can morphology of platelets under a microscope. Bone marrow tests
be identified as small red or purple dots on the skin (Figure 1). may reveal dysfunction in the production and origin of platelets.
Two helpful bone marrow tests are aspiration and biopsy. As-
The nature of illness or mechanism of injury are also import- piration reveals the cause of bone marrow being unable to pro-
ant clues when diagnosing thrombocytopenia. For example, duce blood cells by way of a drawn sample, while a biopsy is the
if a patient suffered from a minor cut or a nosebleed and ex- visual identification of the cells in blood marrow tissue. These
perienced prolonged bleeding, thrombocytopenia should be tests are likely not to be used in a prehospital or emergency/
considered. In female patients, abnormal or prolonged vaginal trauma setting but rather during less acute evaluation when a
bleeding during menstruation can be a sign of a low platelet patient’s platelet count is of concern but not critically low re-
count. Regardless of the cause, heavy bleeding can be serious quiring immediate intervention. Of note, a CBC panel and other
and even fatal, so it is important to monitor blood in the urine laboratory tests often will not be possible to obtain in the field,
or stool as well as the duration and course of any significant so it is critical to quickly identify any signs during the phys-
headaches. ical examination (or from the available history) to determine
Prehospital Treatment of Thrombocytopenia | 77