Page 121 - JSOM Winter 2018
P. 121
Collating and reporting annually will allow us to formulate a no significance in correlation with prehospital lactate levels
training plan directed to these specific needs, to teach the rele- (p=0.8102). The group of patients with TIC and hyperfibrino-
vant core surgical skills (already identified by civilian human- lysis was at the time of preliminary data evaluation too small
itarian organisations) and to facilitate ongoing re- evaluation, to do sufficient statistics.
modification and enhancement of these competencies, tailor-
ing them to new urgent needs. TABLE 1 P-value of base deficit and lactate in Wilcoxon’s two-
sample test (4)
Morbidity and mortality data can then be reviewed, with clin-
ical responses to appropriate surgical interventions.
Finally, a long-term data review program will allow transition Changes in
from individual/group responses to a broader application to Extem or Fibtem TIC Hyperfibrinolysis ISS ≥ 16
guide medical and surgical response planning and resource al- p-value
location in the face of a wide variety of wartime and humani-
tarian crisis situations. Patients 25 11 4 46
BD 0.0135 0.0356 — 0.1096
Research on Trauma Induced Coagulopathy Lactate 0.4432 0.8102 — 0.3453
Ingeborg Bretschneider, Jürgen Kerschowski, Björn Hossfeld,
Martin Kulla, Julia Riedel, Uta Schmid, Matthias Helm
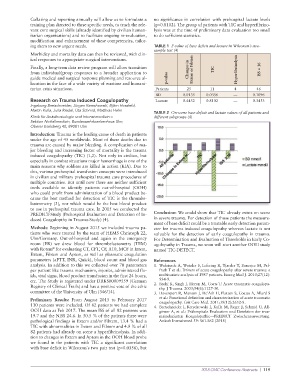
TABLE 2 On-scene base deficit and lactate values of all patients and
Klinik für Anästhesiologie und Intensivmedizin – different subgroups (4)
Sektion Notfallmedizin, Bundeswehrkrankenhaus Ulm,
Oberer Eselsberg 40, 89081 Ulm
Introduction: Trauma is the leading cause of death in patients
under the age of 45 worldwide. Most of these deaths due to
trauma are caused by major bleeding. A complication of ma-
jor bleeding and increasing factor of mortality is the trauma
induced coagulopathy (TIC) (1,2). Not only in civilian, but
especially in combat situations major hemorrhage is one of the
main reasons why soldiers are killed in action (KIA). Due to
this, various prehospital transfusion concepts were introduced
in civilian and military prehospital trauma care procedures of
multiple countries. But until now there are neither sufficient
tools available to identify patients out-of-hospital (OOH)
who could profit from administration of a blood product be-
cause the best method for detection of TIC is the thrombe-
lastrometry (3), nor which would be the best blood product
to use in prehospital trauma care. In 2015 we conducted the
PREDICT-Study (Prehospital Evaluation and Detection of In- Conclusion: We could show that TIC already exists on scene
duced Coagulopthy in Trauma-Study) (4). in severe trauma. For detection of those patients the measure-
ment of base deficit could be a trustable early detection param-
Methods: Beginning in August 2015 we included trauma pa- eter for trauma induced coagulopathy whereas lactate is not
tients who were treated by the team of HEMS Christoph 22, valuable for the detection of early coagulopathy in trauma.
Ulm/Germany. Out-of-hospital and again in the emergency For Determination and Evaluation of Thresholds in Early Co-
room (ER) we drew blood for thrombelastometry (TEM) agulopathy in Trauma, we soon will start another OOH study
with Rotem for evaluating CT, CFT, CF, A10, MCF in Intem, named TIC-DETECT.
®
Extem, Fibtem and Aptem, as well as plasmatic coagulation
parameters (aPTT, INR, Quick), blood count and blood gas References
analysis. In addition to this we collected over 70 parameters 1. Wafaisade A, Wutzler S, Lefering R, Tjardes T, Banerjee M, Paf-
per patient like trauma mechanism, injuries, administered flu- frath T et al.: Drivers of acute coagulopathy after severe trauma: a
ids, vital signs, blood product transfusion in the first 24 hours, multivariate analysis of 1987 patients. Emerg Med J. 2010;27(12):
etc. The Study is registered under DRKS00009559 (German 934-9.
Registry of Clinical Trails) and has a positive vote of the ethic 2. Brohi K, Singh J, Heron M, Coats T: Acute traumatic coagulopa-
thy. J Trauma. 2003;54(6):1127-30.
committee of the University of Ulm (346/14). 3. Davenport R, Manson J, De’Ath H, Platton S, Coates A, Allard S
Preliminary Results: From August 2015 to February 2017 et al.: Functional definition and characterization of acute traumatic
coagulopathy. Crit Care Med. 2011;39(12):2652-8.
130 patients were included. Of 82 patients we had complete 4. Bretschneider I, Kerschowski J, Kulla M, Reger J, Schmid U, All-
OOH data at Feb 2017. The mean ISS of all 82 patients was göwer A, et al.: Prähospitale Evaluation und Detektion der trau-
19.7 and the NISS 24.6. In 30.5 % of the patients there were mainduzierten Koagulopathie—PREDICT Zwischenauswertung.
pathological findings in Extem and/or Fibtem, 13.4 % had a Anästh Intensivmed 59: S61-S62 (2018)
TIC with abnormalities in Extem and Fibtem and 4.9 % of all
82 patients had already on scene a hyperfibrinolysis. In addi-
tion to changes in Extem and Aptem in the OOH blood probe
we found in the patients with TIC a significant correlation
with base deficit in Wilcoxon´s two pair test (p=0.0356), but
2018 CMC Conference Abstracts | 119