Page 99 - Journal of Special Operations Medicine - Fall 2015
P. 99
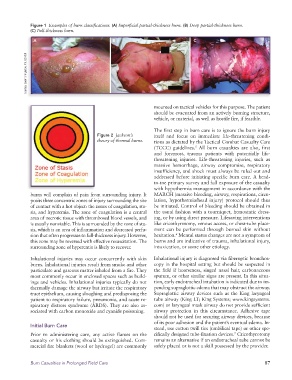
Figure 1 Examples of burn classifications. (A) Superficial partial-thickness burn. (B) Deep partial-thickness burn.
(C) Full-thickness burn.
A B C
Courtesy Sarah Shingleton, RN, USAISR
mounted on tactical vehicles for this purpose. The patient
should be evacuated from an actively burning structure,
vehicle, or material, as well as hostile fire, if feasible.
The first step in burn care is to ignore the burn injury
Figure 2 Jackson’s itself and focus on immediate life-threatening condi-
theory of thermal burns. tions as dictated by the Tactical Combat Casualty Care
(TCCC) guidelines. All burn casualties are also, first
5
and foremost, trauma patients with potentially life-
threatening injuries. Life-threatening injuries, such as
massive hemorrhage, airway compromise, respiratory
insufficiency, and shock must always be ruled out and
addressed before initiating specific burn care. A head-
to-toe primary survey and full exposure of the casualty
with hypothermia management in accordance with the
burns will complain of pain from surrounding injury. It MARCH (massive bleeding, airway, respirations, circu-
posits three concentric zones of injury surrounding the site lation, hypothermia/head injury) protocol should thus
of contact with a hot object: the zones of coagulation, sta- be initiated. Control of bleeding should be obtained in
sis, and hyperemia. The zone of coagulation is a central the usual fashion with a tourniquet, hemostatic dress-
area of necrotic tissue with thrombosed blood vessels, and ing, or by using direct pressure. Lifesaving interventions
is usually nonviable. This is surrounded by the zone of sta- like cricothyrotomy, venous access, or chest-tube place-
sis, which is an area of inflammation and decreased perfu- ment can be performed through burned skin without
sion that often progresses to full-thickness injury. However, hesitation. Mental status changes are not a symptom of
6
this zone may be reversed with effective resuscitation. The burns and are indicative of trauma, inhalational injury,
surrounding zone of hyperemia is likely to recover. intoxication, or some other etiology.
Inhalational injuries may occur concurrently with skin Inhalational injury is diagnosed via fiberoptic bronchos-
burns. Inhalational injuries result from smoke and other copy in the hospital setting but should be suspected in
particulate and gaseous matter inhaled from a fire. They the field if hoarseness, singed nasal hair, carbonaceous
most commonly occur in enclosed spaces such as build- sputum, or other similar signs are present. In this situa-
ings and vehicles. Inhalational injuries typically do not tion, early endotracheal intubation is indicated due to im-
thermally damage the airway but irritate the respiratory pending supraglottic edema that may obstruct the airway.
tract epithelium, causing sloughing and predisposing the Supraglottic airway devices such as the King laryngeal
patient to respiratory failure, pneumonia, and acute re- tube airway (King LT; King Systems; www.kingsystems.
spiratory distress syndrome (ARDS). They are also as- com) or laryngeal mask airway do not provide sufficient
sociated with carbon monoxide and cyanide poisoning. airway protection in this circumstance. Adhesive tape
should not be used for securing airway devices, because
of its poor adhesion and the patient’s eventual edema. In-
Initial Burn Care
stead, use cotton twill ties (umbilical tape) or other spe-
7
Prior to administering care, any active flames on the cifically designed tube-fixation devices. Cricothyrotomy
casualty or his clothing should be extinguished. Com- remains an alternative if an endotracheal tube cannot be
mercial fire blankets (wool or hydrogel) are commonly safely placed or is not a skill possessed by the provider.
Burn Casualties in Prolonged Field Care 87