Page 103 - JSOM Summer 2022
P. 103
9
ventilation allowing a set minimum rate of volume- or pressure- categories: barotrauma, volutrauma, and atelectotrauma.
controlled breaths in conjunction with the patient’s efforts, with These pathologies collectively result in mechanical damage to
the potential for added intermittent assisted breaths to supple- the lung and release of inflammatory mediators further exac-
ment the respiratory requirements of the patient. erbating lung injury. Barotrauma occurs with high mean air-
way pressures during ventilation. PPV at relatively high tidal
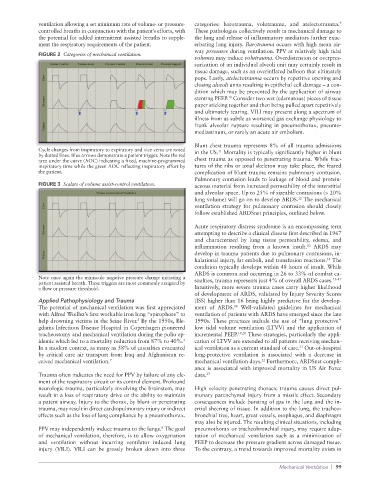
FIGURE 2 Categories of mechanical ventilation.
volumes may induce volutrauma. Overdistension or overpres-
surization of an individual alveoli unit may certainly result in
tissue damage, such as an overinflated balloon that ultimately
pops. Lastly, atelectotrauma occurs by repetitive opening and
closing alveoli units resulting in epithelial cell damage – a con-
dition which may be prevented by the application of airway
stenting PEEP. Consider two wet (edematous) pieces of tissue
10
paper sticking together and then being pulled apart repetitively
and ultimately tearing. VILI may present along a spectrum of
illness from as subtle as worsened gas exchange physiology to
frank alveolar rupture resulting in pneumothorax, pneumo-
mediastinum, or rarely an acute air embolism.
Blunt chest trauma represents 8% of all trauma admissions
Cycle changes from inspiratory to expiratory and vice versa are noted in the US. Mortality is typically significantly higher in blunt
11
by dotted lines. Blue arrows demonstrate a patient trigger. Note the red
area under the curve (AOC) indicating a fixed, machine- programmed chest trauma as opposed to penetrating trauma. While frac-
inspiratory time while the green AOC reflecting inspiratory effort by tures of the ribs or axial skeleton may take place, the feared
the patient. complication of blunt trauma remains pulmonary contusion.
Pulmonary contusion leads to leakage of blood and protein-
FIGURE 3 Scalars of volume assist-control ventilation. aceous material from increased permeability of the interstitial
and alveolar space. Up to 25% of sizeable contusions (> 20%
lung volume) will go on to develop ARDS. The mechanical
12
ventilation strategy for pulmonary contusion should closely
follow established ARDSnet principles, outlined below.
Acute respiratory distress syndrome is an encompassing term
attempting to describe a clinical disease first described in 1967
and characterized by lung tissue permeability, edema, and
13
inflammation resulting from a known insult. ARDS may
develop in trauma patients due to pulmonary contusions, in-
14
halational injury, fat emboli, and transfusion reactions. The
condition typically develops within 48 hours of insult. While
ARDS is common and occurring in 26 to 33% of combat ca-
Note once again the miniscule negative pressure change initiating a sualties, trauma represents just 4% of overall ARDS cases. 15–17
patient assisted breath. These triggers are most commonly assigned by
a flow or pressure threshold. Intuitively, more severe trauma cases carry higher likelihood
of development of ARDS, validated by Injury Severity Scores
Applied Pathophysiology and Trauma (ISS) higher than 16 being highly predictive for the develop-
18
The potential of mechanical ventilation was first appreciated ment of ARDS. Well-validated guidelines for mechanical
with Alfred Woillez’s first workable iron lung “spirophore” to ventilation of patients with ARDS have emerged since the late
help drowning victims in the Seine River. By the 1950s, Ble- 1990s. These practices include the use of “lung protective”
5
gdams Infectious Disease Hospital in Copenhagen pioneered low tidal volume ventilation (LTVV) and the application of
tracheostomy and mechanical ventilation during the polio ep- incremental PEEP. 19,20 These strategies, particularly the appli-
idemic which led to a mortality reduction from 87% to 40%. cation of LTVV are extended to all patients receiving mechan-
6
In a modern context, as many as 58% of casualties evacuated ical ventilation as a current standard of care. Out-of-hospital
21
by critical care air transport from Iraq and Afghanistan re- lung-protective ventilation is associated with a decrease in
ceived mechanical ventilation. 7 mechanical ventilation days. Furthermore, ARDSnet compli-
22
ance is associated with improved mortality in US Air Force
Trauma often indicates the need for PPV by failure of any ele- data. 23
ment of the respiratory circuit or its control element. Profound
neurologic trauma, particularly involving the brainstem, may High velocity penetrating thoracic trauma causes direct pul-
result in a loss of respiratory drive or the ability to maintain monary parenchymal injury from a missile effect. Secondary
a patent airway. Injury to the thorax, by blunt or penetrating consequences include bursting of gas in the lung and the in-
trauma, may result in direct cardiopulmonary injury or indirect ertial sheering of tissue. In addition to the lung, the tracheo-
effects such as the loss of lung compliance by a pneumothorax. bronchial tree, heart, great vessels, esophagus, and diaphragm
may also be injured. The resulting clinical situations, including
PPV may independently induce trauma to the lungs. The goal pneumothorax or tracheobronchial injury, may require adap-
8
of mechanical ventilation, therefore, is to allow oxygenation tation of mechanical ventilation such as a minimization of
and ventilation without incurring ventilator induced lung PEEP to decrease the pressure gradient across damaged tissue.
injury (VILI). VILI can be grossly broken down into three To the contrary, a trend towards improved mortality exists in
Mechanical Ventilation | 99